What Are Your Toric IOL Options?
A toric IOL is a specialized artificial lens implanted during cataract surgery that corrects corneal astigmatism by incorporating different focusing powers along different meridians of the lens. Unlike standard IOLs with uniform power, toric designs neutralize the eye’s irregular curvature at its source.
This guide covers toric IOL types and how they compare, candidacy and potential risks, surgical expectations and newer technologies, and costs and insurance realities.
Three distinct toric IOL categories are available in 2026: monofocal toric lenses optimized for sharp single-distance vision, multifocal toric lenses designed to reduce spectacle dependence across near, intermediate, and far distances, and EDOF toric lenses that stretch a continuous focal range with fewer optical side effects than multifocal designs. Each category pairs astigmatism correction with a different approach to functional vision range.
Candidacy depends on factors like astigmatism severity, corneal regularity, and overall ocular health. Certain conditions, including irregular astigmatism and zonular instability, may make toric implantation unsuitable. Rotational stability and residual astigmatism remain the primary clinical concerns, though modern lens materials and AI-optimized calculation formulas have narrowed the gap between predicted and actual outcomes considerably.
The surgical process involves precise preoperative biometry, a brief implantation procedure, and a structured recovery period with follow-up visits to verify lens alignment. Newer technologies, including advanced hydrophobic acrylic platforms and post-operative light-adjustable correction, continue to refine results.
Out-of-pocket costs vary by lens type, lower for monofocal toric upgrades and higher for multifocal toric options. Medicare covers standard cataract removal, but premium toric lenses typically require an incremental patient payment.
What Is a Toric IOL and How Does It Correct Astigmatism?
A toric IOL is a specialized artificial lens implanted during cataract surgery to correct corneal astigmatism. It works by incorporating different focusing powers in different meridians of the lens, compensating for the eye’s irregular curvature.
Unlike a standard IOL that has uniform power across its surface, a toric IOL features a specific cylindrical correction built into its design. This asymmetric optical profile aligns with the steeper and flatter axes of an astigmatic cornea, neutralizing the refractive error at its source. According to StatPearls (NCBI Bookshelf), toric intraocular lenses correct corneal astigmatism by incorporating different focusing powers in different parts of the lens, replacing the clouded natural lens and the astigmatism correction in a single procedure.
Precise rotational alignment is critical for toric IOL performance. Even small degrees of misalignment can reduce the intended astigmatism correction, which is why surgeons use advanced preoperative imaging and intraoperative guidance systems to position the lens accurately. Newer technologies continue to refine this process. The Light Adjustable Lens, for example, allows up to 2.5 diopters of post-operative astigmatism correction using controlled ultraviolet light after healing, though it requires additional follow-up visits.
For patients with regular corneal astigmatism undergoing cataract removal, toric IOLs remain one of the most practical single-step solutions available. The sections ahead explore candidacy requirements, the three main toric IOL categories, and how each type addresses different visual needs.
Who Is a Good Candidate for a Toric IOL in 2026?
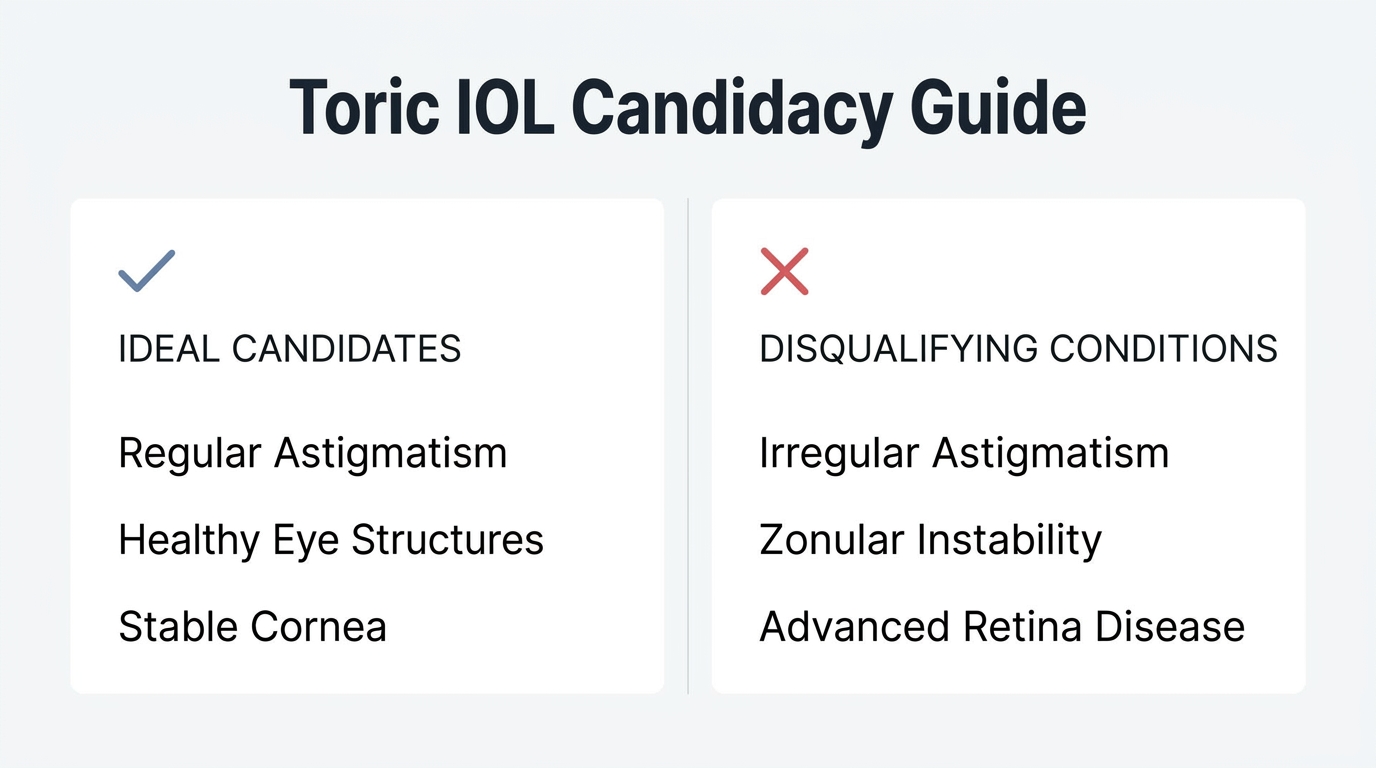
A good candidate for a toric IOL in 2026 typically has regular corneal astigmatism of 1.0 D or more and healthy ocular structures. The sections below cover the astigmatism thresholds that may benefit from toric correction and the eye conditions that might disqualify a patient.
What Level of Astigmatism May Benefit From a Toric IOL?
According to the European Society of Cataract and Refractive Surgeons (ESCRS) 2024 guidelines, toric IOLs should be considered in eyes with corneal astigmatism of 1.0 D or more. Patients with lower amounts of astigmatism may still notice blurred or distorted vision, but the corrective benefit of a toric lens becomes more measurable and visually significant at this threshold. For higher levels of astigmatism, toric IOLs can provide even greater reductions in spectacle dependence after cataract surgery.
Patient awareness also plays a role in outcomes. John A. Hovanesian, MD, at Harvard Eye Associates notes that he begins toric IOL consultations by asking whether patients understand their astigmatism diagnosis, allowing him to tailor the conversation to their knowledge level. This kind of preoperative communication helps set realistic expectations, which is just as important as the clinical measurements themselves.
What Eye Conditions Might Disqualify You From a Toric IOL?
The eye conditions that might disqualify you from a toric IOL include irregular astigmatism, zonular instability, and pre-existing posterior segment pathology. According to StatPearls (NIH), these conditions can compromise both the rotational stability and visual performance of a toric lens.
Key disqualifying conditions include:
- Irregular astigmatism caused by corneal scarring or prior refractive surgery, where the corneal surface is too unpredictable for standard toric correction.
- Zonular instability, which may prevent the IOL from maintaining its intended alignment inside the capsular bag.
- Posterior segment pathology, such as advanced macular degeneration or significant diabetic retinopathy, where the retina limits the visual benefit regardless of lens choice.
- Uncontrolled glaucoma or active ocular inflammation, which can complicate surgery and recovery.
Candidates with any of these conditions may benefit from alternative approaches. A thorough preoperative evaluation, including corneal topography and biometry, helps the surgeon determine whether toric correction is appropriate or whether a different lens strategy would yield better results.
Understanding candidacy criteria is the first step; the next section explores the specific types of toric IOLs available in 2026.

What Are the Types of Toric IOLs Available in 2026?
The types of toric IOLs available in 2026 are monofocal toric, multifocal toric, and extended depth of focus (EDOF) toric. Each design corrects corneal astigmatism during cataract surgery while offering a different range of functional vision.

Monofocal Toric IOL
A monofocal toric IOL is a single-focus lens that corrects astigmatism at one set distance, typically optimized for clear distance vision. Because the lens provides only one focal point, most patients still need reading glasses for near tasks after surgery.
This design suits patients who prioritize sharp, high-contrast distance vision with minimal optical side effects. Monofocal toric lenses generally produce fewer visual disturbances, such as halos and glare, compared to multifocal designs. That predictability makes them a reliable choice for individuals with straightforward visual needs or those who already wear readers comfortably.
For patients whose primary concern is reducing dependence on distance glasses while managing astigmatism, the monofocal toric IOL remains one of the most well-established options available.
Multifocal Toric IOL
A multifocal toric IOL is a lens that corrects astigmatism while providing multiple focal points for distance, intermediate, and near vision. The goal is to reduce or eliminate the need for glasses across most daily activities. This makes them a popular choice among those seeking lifestyle-based vision correction.
According to a prospective study published in Medical Hypothesis, Discovery & Innovation in Ophthalmology, 93.9% and 90.2% of patients with bilateral trifocal IOL implantation reported complete spectacle independence for distance and near vision, respectively, at six months postoperatively. These results illustrate the potential of multifocal toric technology for patients seeking broad visual freedom.
The trade-off involves a higher likelihood of visual phenomena, such as halos around lights and mild glare, particularly in low-light conditions. Patients with demanding nighttime driving needs should weigh this carefully with their surgeon before committing to a multifocal toric design.
Extended Depth of Focus Toric IOL
An extended depth of focus (EDOF) toric IOL is a lens that corrects astigmatism while elongating the range of clear vision from distance through intermediate without splitting light into distinct focal points. Rather than creating separate zones for near and far, the EDOF design stretches a single continuous focal zone.
This approach typically produces fewer halos and less glare than multifocal designs, making it appealing for patients sensitive to nighttime visual disturbances. Intermediate tasks, such as computer work and cooking, tend to remain comfortable without glasses. However, near vision for fine print may still require reading glasses in some cases.
EDOF toric lenses occupy a practical middle ground between the simplicity of monofocal toric and the full range of multifocal toric designs. For patients who want broader functional vision than a monofocal offers but fewer optical compromises than a multifocal demands, the EDOF toric IOL often represents a well-balanced option.
With each toric IOL type offering distinct visual trade-offs, understanding how they compare in detail helps guide the right choice.
How Does a Monofocal Toric IOL Differ From a Standard Monofocal?
A monofocal toric IOL differs from a standard monofocal by adding built-in astigmatism correction to the single-focus lens design. The sections below cover expected vision range and ideal candidacy scenarios.
What Range of Vision Can You Expect With a Monofocal Toric IOL?
The range of vision you can expect with a monofocal toric IOL is optimized for one focal point, typically distance, with significantly reduced astigmatism compared to a standard monofocal lens. Reading glasses remain necessary for near and intermediate tasks.
What distinguishes this lens is its rotational stability, which directly determines how well astigmatism correction holds over time. According to a 2025 retrospective study of 161 eyes published in Clinical Ophthalmology, the Clareon aspheric monofocal toric IOL demonstrated a mean absolute rotation of just 1.02 ± 1.21° at one month post-surgery, with 70.1% of eyes achieving residual astigmatism of 0.25 D or less.
For patients whose primary goal is crisp distance vision without the optical trade-offs of multifocal designs, monofocal toric IOLs can deliver exceptionally clean visual quality. The single-focus optic avoids light-splitting, which means halos and glare are typically minimal. This makes the monofocal toric one of the most predictable toric IOL options for patients who are comfortable wearing reading glasses.
When Might a Monofocal Toric IOL Be the Best Choice?
A monofocal toric IOL may be the best choice when a patient has regular corneal astigmatism and prioritizes sharp distance vision with minimal visual disturbances. Several clinical scenarios favor this lens:
- Patients who already wear reading glasses comfortably and want clear unaided distance vision after cataract surgery.
- Individuals with occupations requiring high-contrast visual acuity, such as night driving or precision work, where halos and glare from multifocal optics could be problematic.
- Patients with pre-existing ocular conditions, such as mild macular changes, that may limit the benefits of multifocal or EDOF designs.
- Those seeking a lower out-of-pocket premium compared to multifocal toric or EDOF toric lenses.
In clinical practice, the monofocal toric IOL is often the most reliable starting recommendation for patients new to premium lens discussions. Its straightforward optical design reduces the variables that can affect satisfaction, making it a strong foundation for managing expectations.
With the monofocal toric’s strengths defined, multifocal toric IOLs expand the conversation to presbyopia correction alongside astigmatism.
How Does a Multifocal Toric IOL Address Both Astigmatism and Presbyopia?
A multifocal toric IOL addresses both astigmatism and presbyopia by combining astigmatism-correcting cylinder power with multiple focal zones that restore near, intermediate, and distance vision. The following subsections cover expected vision range, possible side effects, and ideal candidacy.
What Range of Vision Can You Expect With a Multifocal Toric IOL?
The range of vision you can expect with a multifocal toric IOL spans distance, intermediate, and near focal points. The toric component corrects corneal astigmatism, while the multifocal optic splits incoming light into separate focus zones. This design may allow many patients to perform most daily tasks, from driving to reading, with reduced dependence on glasses.
Because light is divided among multiple focal points, contrast sensitivity can be slightly lower than with a monofocal toric lens, particularly in dim lighting. Patients with high visual demands at a single distance may notice this trade-off. Still, for those seeking broad spectacle independence alongside astigmatism correction, the multifocal toric platform represents one of the most practical options available in 2026.
What Visual Side Effects Are Possible With a Multifocal Toric IOL?
The visual side effects possible with a multifocal toric IOL include halos, glare, and starbursts around lights, especially at night. These photic phenomena result from the lens splitting light across multiple focal zones. Most patients find that these symptoms diminish over several weeks as the brain adapts through neuroadaptation, though some individuals remain more sensitive long-term.
Candidacy screening helps minimize risk. According to StatPearls (NIH), toric IOLs are considered unsuitable for patients with pre-existing posterior segment pathology, zonular instability, or irregular astigmatism, as these conditions can compromise lens stability and visual performance. Patients with unrealistic expectations for perfect night vision or those who drive extensively in low-light conditions should discuss these trade-offs thoroughly with their ophthalmologist before choosing a multifocal design.
When Might a Multifocal Toric IOL Be the Best Choice?
A multifocal toric IOL may be the best choice when a patient has both clinically significant corneal astigmatism and presbyopia, and desires broad spectacle independence across all distances. Ideal candidates typically include individuals who:
- Have regular corneal astigmatism of 1.0 D or greater, the threshold at which the ESCRS 2024 guidelines recommend considering toric correction.
- Want to minimize reliance on reading glasses and distance glasses after cataract surgery.
- Have healthy retinas and stable ocular anatomy with no irregular astigmatism or zonular weakness.
- Accept that mild halos or glare may occur during the neuroadaptation period.
Patients with ocular comorbidities or those who prioritize crisp single-distance vision over range may find a monofocal toric or EDOF toric lens more suitable. Understanding how EDOF toric technology compares can further clarify which platform best fits your visual goals.
How Does an EDOF Toric IOL Compare to a Multifocal Toric IOL?
An EDOF toric IOL compares to a multifocal toric IOL by offering a continuous, elongated focal range rather than splitting light into distinct near, intermediate, and distance zones. The sections below cover expected vision range, side effects, and ideal candidacy.

What Range of Vision Can You Expect With an EDOF Toric IOL?
The range of vision you can expect with an EDOF toric IOL is a seamless corridor from distance through intermediate, with functional near capability. Unlike multifocal toric designs that create separate focal points for reading, computer, and driving distances, an EDOF toric lens stretches a single focus across a broader depth of field.
This design typically delivers excellent distance and intermediate clarity, making tasks like computer work, cooking, and dashboard reading comfortable without glasses. Near vision for fine print may still require occasional reading glasses, though the gap is narrower than with a monofocal toric. For patients who prioritize smooth transitions between distances over maximum reading independence, this extended range often represents the most natural-feeling visual experience among premium toric options.
What Visual Side Effects Are Possible With an EDOF Toric IOL?
The visual side effects possible with an EDOF toric IOL include halos, glare, and starbursts around lights at night, though these tend to be milder than those reported with multifocal toric designs. Because EDOF lenses elongate the focal point rather than splitting light into multiple rings, less light energy is diverted away from the primary image.
Some patients notice mild contrast sensitivity reduction in low-light conditions, particularly during the neuroadaptation period in the first few weeks after surgery. These symptoms generally diminish as the brain adjusts to the new optical profile. Patients with large pupils or those who drive frequently at night should discuss these potential effects with their ophthalmologist beforehand. In clinical practice, EDOF toric lenses consistently produce fewer bothersome nighttime visual disturbances than their multifocal counterparts, which makes them a compelling option for patients sensitive to optical artifacts.
When Might an EDOF Toric IOL Be the Best Choice?
An EDOF toric IOL might be the best choice for patients with corneal astigmatism who want reduced spectacle dependence across distance and intermediate tasks while minimizing nighttime visual disturbances. Ideal candidates include:
- Active professionals who spend significant time on computers or digital screens and need reliable intermediate vision.
- Patients bothered by halos and glare who still want more range than a monofocal toric provides.
- Individuals comfortable wearing reading glasses occasionally for prolonged fine-print tasks.
- Patients with mild ocular surface irregularities where a multifocal’s light-splitting design may amplify visual disturbances.
Your ophthalmologist may recommend an EDOF toric over a multifocal toric when lifestyle priorities favor visual quality and smooth transitions rather than maximum near independence. Understanding how each premium lens category addresses astigmatism and presbyopia can help clarify the remaining factors to consider, including potential risks.
What Are the Potential Risks and Complications of Toric IOLs?
The potential risks and complications of toric IOLs include postoperative lens rotation and residual astigmatism. These two issues represent the most clinically significant concerns specific to toric lens implantation.
What Happens if a Toric IOL Rotates After Surgery?
If a toric IOL rotates after surgery, the astigmatism correction becomes misaligned with the corneal axis, which can reduce visual clarity. Because toric lenses rely on precise axis alignment to neutralize corneal astigmatism, even small degrees of rotation may diminish the refractive benefit. A 2025 retrospective study of 161 eyes published in Clinical Ophthalmology found that the Clareon aspheric monofocal toric IOL demonstrated a mean absolute rotation of only 1.02 ± 1.21° at one month post-surgery. Modern lens designs with enhanced haptic stability have significantly reduced this risk, though rotation beyond approximately 10 degrees may require surgical repositioning. Lens rotation is one of the most overestimated risks patients worry about; current-generation toric IOLs maintain remarkably stable alignment in the vast majority of cases.
Can Residual Astigmatism Occur After Toric IOL Implantation?
Yes, residual astigmatism can occur after toric IOL implantation. Small amounts of uncorrected astigmatism may remain due to factors such as posterior corneal astigmatism, slight lens misalignment, or variability in preoperative measurements. Still, outcomes have improved considerably with modern biometry. AI-optimized IOL power calculation formulas, such as the Kane formula and Barrett Universal II, have reduced mean absolute error to approximately 0.25–0.30 D according to a 2026 report in The Ophthalmologist, improving toric IOL selection accuracy. For patients who do experience clinically meaningful residual astigmatism, options such as lens repositioning, laser enhancement, or the Light Adjustable Lens may help refine the result. Residual astigmatism is rarely severe enough to compromise daily function, but discussing realistic expectations with your ophthalmologist before surgery remains essential.
With these risks in perspective, understanding toric IOL costs helps complete the decision-making picture.
How Much Do Toric IOLs Cost in 2026?
Toric IOL costs in 2026 depend on the lens type selected. Monofocal toric, multifocal toric, and EDOF toric IOLs each carry different out-of-pocket upgrade fees beyond what insurance covers.
How Much Does a Monofocal Toric IOL Typically Cost?
A monofocal toric IOL typically costs between $1,000 and $1,500 per eye as an out-of-pocket upgrade fee. According to a 2026 Medicare coverage guide published by Karschner Insurance, Medicare Part B covers the cost of medically necessary cataract removal with a standard monofocal IOL, but patients choosing premium lenses such as toric models are typically responsible for the incremental upgrade amount.
This means the surgical procedure itself and a basic lens may be covered, while the astigmatism-correcting component remains a patient expense. Private insurance plans generally follow a similar structure. For patients with moderate corneal astigmatism who primarily need sharp distance vision, the monofocal toric upgrade often represents the most cost-effective premium lens investment.
How Much Does a Multifocal Toric IOL Typically Cost?
A multifocal toric IOL typically costs more than a monofocal IOL per eye as an out-of-pocket upgrade. The higher price reflects the lens’s dual correction capability: it addresses both corneal astigmatism and presbyopia within a single implant.
Because multifocal toric lenses incorporate complex optical zones for distance, intermediate, and near vision, their manufacturing costs exceed those of simpler toric designs. Facility fees, surgeon experience, and geographic location can also influence the final price. Patients should request an itemized quote from their surgical center, as some practices bundle pre-operative diagnostics and post-operative visits into the total fee while others bill separately.
How Much Does an EDOF Toric IOL Typically Cost?
An EDOF toric IOL typically costs between the price of a monofocal and multifocal IOL per eye as an out-of-pocket upgrade. This price point falls between monofocal toric and multifocal toric lenses, reflecting the EDOF design’s elongated focal range without the multiple distinct focal points of a multifocal.
Many patients find EDOF toric pricing attractive because it offers a broader range of functional vision than a monofocal toric at a lower cost than most multifocal toric options. Flexible spending accounts, health savings accounts, and interest-free payment plans offered by many surgical practices can help manage these expenses. Your ophthalmologist can provide a personalized cost estimate based on your specific lens selection and insurance coverage.
With costs clarified, understanding what to expect before, during, and after surgery helps you prepare fully.

What Should You Expect Before, During, and After Toric IOL Surgery?
You should expect a structured process that includes precise pre-operative measurements, a brief surgical procedure, and a recovery period with scheduled follow-up visits.
Before surgery, your ophthalmologist performs detailed biometric measurements to determine the correct toric IOL power and axis alignment. AI-optimized IOL power calculation formulas, such as the Kane formula and Barrett Universal II, have reduced mean absolute error to approximately 0.25–0.30 D according to a 2026 report in The Ophthalmologist, improving the precision of toric lens selection. Corneal topography maps the exact shape and curvature of your cornea, while optical biometry measures axial length. Your surgeon may also place alignment marks on the cornea to guide lens positioning.
During surgery, cataract removal and toric IOL implantation typically take 10 to 20 minutes per eye under local anesthesia. The surgeon removes the clouded natural lens through a small incision, then inserts the toric IOL and rotates it to the predetermined axis. Precise rotational alignment is critical because even small degrees of misalignment can reduce the astigmatism-correcting benefit.
After surgery, most patients notice improved clarity within the first few days, though full visual stabilization may take several weeks. Post-operative visits allow your ophthalmologist to verify that the lens has remained rotationally stable and that residual astigmatism falls within the target range. Prescribed eye drops help manage inflammation and prevent infection during healing.
From a practical standpoint, the preoperative measurement phase is arguably the most important step in the entire process. Patients who invest time in thorough consultations and advanced biometry tend to achieve the most predictable outcomes. Understanding what each phase involves can help you prepare for the next step: exploring how newer toric IOL technologies in 2026 may further improve results.
How Do Newer Toric IOL Technologies in 2026 Improve Outcomes?
Newer toric IOL technologies in 2026 improve outcomes through AI-optimized lens calculations, advanced material platforms with superior rotational stability, and post-operative adjustment capabilities. These advances reduce residual astigmatism and increase spectacle independence across all toric IOL categories.
AI-optimized IOL power calculation formulas represent one of the most significant advances shaping toric lens selection today. According to a 2026 report in The Ophthalmologist, formulas such as the Kane formula and Barrett Universal II have reduced mean absolute error to approximately 0.25–0.30 D, substantially improving the precision of toric IOL power selection. More accurate preoperative calculations translate directly into fewer refractive surprises after surgery.
Material science has also advanced considerably. Newer hydrophobic acrylic platforms, like the Clareon material used in Alcon’s latest toric models, demonstrate exceptional rotational stability. When a toric IOL stays precisely aligned on its intended axis, the astigmatism correction remains effective long term. Even small improvements in lens stability can meaningfully reduce the need for secondary repositioning procedures.
Post-operative adjustability is another emerging capability. The Light Adjustable Lens allows up to 2.5 D of astigmatism correction using controlled ultraviolet light after the eye has healed, though it requires additional follow-up visits for adjustment. This technology shifts part of the refractive fine-tuning from the operating room to the postoperative period, offering a safety net for patients whose final refractive outcome differs slightly from the surgical target.
For patients and surgeons alike, these converging innovations make 2026 a particularly promising year for toric IOL outcomes. Understanding which technologies align with your specific visual needs is the next step toward making a confident lens choice.
How Can Cataract Surgery Education Help You Choose the Right Toric IOL?
Cataract surgery education can help you choose the right toric IOL by providing clear, unbiased guidance on lens types, costs, and candidacy. The sections below cover how Eye Surgery Today supports your decision-making and the key takeaways for 2026.
Can Eye Surgery Today Help You Understand Your Toric IOL Options?
Yes, Eye Surgery Today can help you understand your toric IOL options. As an education platform founded by nationally recognized ophthalmology key opinion leaders, Eye Surgery Today translates complex surgical concepts into clear, accessible language. The platform provides comprehensive guides covering monofocal toric, multifocal toric, and EDOF toric IOLs, including candidacy criteria, expected visual outcomes, and cost considerations.
Choosing between toric IOL categories involves weighing factors that vary by patient. Understanding insurance coverage is one common concern; in 2026, Medicare Part B covers medically necessary cataract removal with a standard monofocal IOL, but patients selecting premium lenses like toric or multifocal options are typically responsible for the incremental upgrade cost. Eye Surgery Today breaks down these financial realities alongside clinical data so patients can approach their ophthalmologist prepared with informed questions rather than uncertainty.
What Are the Key Takeaways About Toric IOL Options in 2026?
The key takeaways about toric IOL options in 2026 center on improved precision, expanded lens categories, and the importance of informed decision-making. Three main toric IOL types serve distinct visual needs:
- Monofocal toric IOLs correct astigmatism while providing sharp distance vision, though reading glasses remain necessary.
- Multifocal toric IOLs address astigmatism and presbyopia simultaneously, offering distance and near vision with a higher risk of visual side effects such as halos and glare.
- EDOF toric IOLs provide a continuous range of focus from distance through intermediate with fewer optical disturbances than multifocal designs.
Lens selection accuracy has also advanced considerably. According to a 2026 report in The Ophthalmologist, AI-optimized IOL power calculation formulas such as the Kane formula and Barrett Universal II have reduced mean absolute error to approximately 0.25 to 0.30 D, improving toric IOL selection precision. For most patients, this means the gap between predicted and actual outcomes continues to narrow, making the pre-operative conversation with your surgeon more important than ever.
With a clearer understanding of these options, discussing your visual goals and lifestyle priorities with your ophthalmologist can help identify the toric IOL best suited to your needs.