Why Is Cataract Surgery Considered Pain-Free and Safe?
Cataract surgery is a procedure that removes the eye’s clouded natural lens and replaces it with an artificial intraocular lens (IOL) to restore vision. In 2026, layered anesthesia protocols and precision surgical technology have made it one of the most well-tolerated procedures in modern medicine.
This guide covers pain management and anesthesia approaches, surgical technologies that enhance safety, complication rates and risks, the step-by-step patient experience, candidacy and recovery, and how informed preparation can build confidence before surgery day.
Modern anesthesia combines topical numbing drops, intracameral lidocaine injected into the anterior chamber, and optional mild sedation to address both surface and internal sensation. Patients may still feel mild pressure or light sensitivity, but sharp pain is not expected under this layered approach.
Femtosecond laser-assisted systems, advanced phacoemulsification platforms, and real-time intraoperative OCT imaging allow surgeons to automate delicate steps with micron-level accuracy while monitoring tissue layers beneath the surgical field. These tools may reduce ultrasound energy requirements and thermal stress on surrounding structures.
Serious complications remain rare. Endophthalmitis incidence ranges from 0.01% to 0.22%, clinically significant cystoid macular edema occurs in approximately 0.82% of routine cases, and posterior capsule opacification, the most common long-term finding, is treatable with a brief in-office laser procedure.
Most patients notice improved vision within the first few days, with initial healing spanning two to four weeks. Driving clearance often comes within the first week, though complete internal healing may continue for several months. Patients with diabetes or glaucoma can typically still qualify after thorough preoperative evaluation.
Understanding each phase of the procedure, from preoperative preparation through recovery milestones, may help replace uncertainty with confidence well before surgery day arrives.
What Makes Modern Cataract Surgery Pain-Free?
Modern cataract surgery is pain-free because of a layered anesthesia approach combining topical numbing drops, intracameral lidocaine, and optional mild sedation. Each layer targets a different source of potential discomfort.
How Do Topical Anesthetic Eye Drops Eliminate Pain?
Topical anesthetic eye drops eliminate pain by blocking nerve signals on the corneal surface before any instrument touches the eye. Drops such as proparacaine, tetracaine, or oxybuprocaine numb the outer tissues within seconds of application. According to a review published in Annals of Emergency Medicine (2024), these commercial topical anesthetics can be safely administered up to every 30 minutes for acute pain management. Because the drops work directly on the cornea, patients avoid the risks associated with needle-based injections around the eye. This surface-level numbing forms the first and most critical layer of the pain-free experience during phacoemulsification.
How Does Intracameral Anesthesia Work During Surgery?
Intracameral anesthesia works by injecting a small amount of lidocaine directly into the anterior chamber of the eye during surgery. This targets the iris and deeper intraocular structures that topical drops alone may not fully reach. According to research published in PMC (2018), intracameral lidocaine supplementing topical anesthesia is a simple, secure method that can increase analgesia and eliminate discomfort during cataract surgery. Surgeons typically inject the lidocaine through the same micro-incision used for the procedure, adding no extra steps. Real-time imaging tools, including intraoperative OCT, further enhance surgical precision throughout this process. For most patients, this dual-layer approach addresses both surface and internal sensation effectively.
Can Mild Sedation Help With Anxiety During the Procedure?
Yes, mild sedation can help with anxiety during the procedure. Oral or intravenous sedatives, such as low-dose midazolam, may be offered to patients who feel nervous before surgery. According to a study published in PMC (2024), preoperative anxiety determining factors include younger age and female gender, with a mean anxiety score of 10.8±5.2. Sedation does not replace local anesthesia; it complements numbing drops and intracameral lidocaine by calming the patient’s overall state. Patients remain awake and responsive but feel relaxed. Discussing anxiety concerns with your ophthalmologist beforehand allows the surgical team to tailor the sedation level appropriately.
What Sensations May You Feel Even With Numbing?
The sensations you may feel even with numbing are mild pressure, slight coolness from irrigating fluid, and occasional light sensitivity. Pain is not expected, but the eye’s deeper proprioceptive nerves can still register touch and pressure sensations that anesthesia does not fully suppress. Some patients describe a gentle pushing feeling when the surgeon removes the cloudy lens. Brief flashes or shifts in light perception are also common as instruments move near the visual axis. These sensations are normal, typically last only seconds, and should not be confused with pain. Knowing what to expect often reduces the surprise factor considerably.
With pain management strategies understood, exploring the full range of anesthesia options helps patients and surgeons choose the best approach together.
What Anesthesia Options Are Available for Cataract Surgery?
The anesthesia options available for cataract surgery include topical eye drops, injection-based nerve blocks, and general anesthesia. Each approach suits different patient needs and clinical scenarios.
How Does Topical Anesthesia Differ From Injection-Based Anesthesia?
Topical anesthesia differs from injection-based anesthesia in delivery method, depth of numbing, and risk profile. Topical anesthesia uses numbing eye drops applied directly to the corneal surface, while injection-based techniques, such as retrobulbar or peribulbar blocks, deliver anesthetic around the eye through a needle to block deeper nerve pathways.
Topical drops allow patients to retain eye movement during surgery, and recovery tends to be faster. However, phacoemulsification with topical anesthesia is not a completely painless procedure; pain intensity can vary with cataract type and the specific surgical stage. Adding intracameral lidocaine inside the eye significantly reduces discomfort. According to a study published in PubMed, patients report significantly less pain with combined topical and intracameral lidocaine compared to topical anesthesia alone (P = .001).
Injection-based blocks provide more complete numbing and temporary eye immobilization, which some surgeons prefer for complex cases. For most routine procedures, topical anesthesia with intracameral supplementation offers an effective, lower-risk alternative.
When May a Retrobulbar or Peribulbar Block Be Recommended?
A retrobulbar or peribulbar block may be recommended when deeper anesthesia and complete eye immobilization are clinically necessary. These injection-based techniques deliver anesthetic around the orbital nerves, temporarily paralyzing eye movement.
Situations where surgeons may prefer a regional block include:
- Dense or mature cataracts requiring longer surgical time.
- Patients unable to remain still or follow instructions during the procedure.
- Cases involving significant ocular inflammation or trauma.
- Complicated procedures combined with additional interventions, such as glaucoma surgery.
Peribulbar blocks carry a slightly lower risk of complications than retrobulbar blocks because the needle stays outside the muscle cone. Both techniques remain safe and well-established when performed by experienced practitioners. In clinical practice, regional blocks are increasingly reserved for complex cases, since topical approaches handle most routine surgeries effectively.
Is General Anesthesia Ever Used for Cataract Surgery?
General anesthesia is rarely used for cataract surgery, but it may be appropriate in specific circumstances. Most cataract procedures rely on local anesthetic techniques because they carry fewer systemic risks and allow faster recovery.
Situations where general anesthesia may be considered include:
- Young children undergoing pediatric cataract removal.
- Patients with severe anxiety disorders unresponsive to sedation.
- Individuals unable to lie still due to tremors, movement disorders, or cognitive impairment.
- Cases where local anesthesia is medically contraindicated.
Non-pharmacological strategies can also help manage anxiety. According to a 2024 study published in ScienceDirect, patients undergoing cataract surgery with music intervention experience a significant decrease in pain levels (SMD −0.74), suggesting supportive measures may reduce the need for deeper sedation. General anesthesia remains a safe option when needed, though its use adds complexity and requires careful preoperative evaluation.
With anesthesia options tailored to each patient, the next consideration is the surgical technology that enhances safety.
What Technologies Help Make Cataract Surgery Safer in 2026?
Technologies that help make cataract surgery safer in 2026 include femtosecond laser systems, advanced phacoemulsification platforms, intraoperative aberrometry, and real-time OCT guidance.
How Does Femtosecond Laser-Assisted Surgery Improve Precision?
Femtosecond laser-assisted surgery improves precision by automating the most delicate steps of cataract removal, including corneal incisions, capsulotomy creation, and lens fragmentation. The laser creates incisions with micron-level accuracy that manual blades cannot consistently replicate.
According to a meta-analysis of 46 randomized controlled trials involving 8,871 eyes published in PMC, femtosecond laser-assisted cataract surgery (FLACS) yielded significantly better corrected distance visual acuity one week postoperatively (P = 0.011) compared to conventional techniques. Pre-fragmenting the lens with laser energy also reduces the ultrasound power needed during subsequent phacoemulsification, which may lower thermal stress on surrounding tissue. For patients with dense cataracts, this combination of laser precision and reduced energy delivery represents one of the most meaningful advances in surgical safety.
How Do Advanced Phacoemulsification Systems Reduce Risk?
Advanced phacoemulsification systems reduce risk by using real-time power modulation and smaller incision profiles to minimize intraocular trauma during lens removal. Modern platforms automatically adjust vacuum, flow rate, and ultrasound energy in response to changing tissue resistance.
These adaptive systems help maintain stable anterior chamber depth throughout the procedure, reducing the likelihood of posterior capsule rupture. Torsional and transversal ultrasound modes generate less heat at the incision site than traditional longitudinal phacoemulsification, which may decrease the risk of thermal corneal burns. Surgeons benefit from greater control during the most technically demanding phases of nucleus removal, particularly in cases involving hard or brunescent cataracts where excessive energy was previously unavoidable.
How Does Intraoperative Aberrometry Enhance Outcomes?
Intraoperative aberrometry enhances outcomes by measuring the eye’s refractive state in real time during surgery, allowing surgeons to verify or adjust intraocular lens (IOL) power selection before closing. The ORA System is one widely used wavefront aberrometry platform for this purpose.
However, the technology has notable limitations. According to a study published in Nature Scientific Reports, intraoperative aberrometry using the ORA system for IOL power calculation does not provide reliable refraction results in some clinical settings compared to preoperative biometry. This finding highlights that aberrometry works best as a confirmatory tool alongside thorough preoperative measurements rather than a standalone replacement. When used to cross-check biometry calculations, particularly in post-refractive surgery eyes or eyes with irregular corneas, it can still add a valuable layer of verification.
How Does Real-Time OCT Guidance Improve Surgical Safety?
Real-time OCT guidance improves surgical safety by providing depth-resolved, cross-sectional imaging of intraocular structures while the surgeon operates. Intraoperative optical coherence tomography (iOCT) displays live tissue layers, enabling visualization of anatomy that is otherwise hidden beneath the surgical field.
This technology allows surgeons to confirm wound architecture, assess lens fragment positioning, and detect complications such as Descemet membrane detachments during the procedure itself. Rather than relying solely on the surgical microscope’s surface view, iOCT reveals subsurface detail in real time. The added imaging layer is especially valuable in complex cases where tissue planes are difficult to distinguish visually.
With these technologies working together, the next consideration is understanding what risks remain even with modern surgical advances.
What Are the Possible Risks and Complications of Cataract Surgery?
The possible risks and complications of cataract surgery include posterior capsule opacification, endophthalmitis, cystoid macular edema, retinal detachment, and residual refractive error. Each complication occurs at a low rate, as the sections below detail.

How Common Is Posterior Capsule Opacification After Surgery?
Posterior capsule opacification after surgery is the most frequently reported long-term complication, though its incidence remains low. PCO occurs when residual lens epithelial cells proliferate across the posterior capsule, causing secondary visual clouding months or years after the initial procedure.
A 2022 report covering 500,872 eyes found the incidence of PCO six months after surgery to be 2.3%. When treatment becomes necessary, Nd:YAG posterior capsulotomy resolves the condition quickly. According to a meta-analysis of 129 studies published in PubMed, the incidence of Nd:YAG capsulotomy is approximately 0.5%, suggesting that most PCO cases remain clinically insignificant.
Because the fix is a brief, noninvasive laser procedure performed in an office setting, PCO is widely considered the most manageable complication of cataract surgery.
What Is the Risk of Endophthalmitis After Cataract Surgery?
The risk of endophthalmitis after cataract surgery is very low, with reported incidence rates ranging from 0.01% to 0.22% across countries and study populations. Endophthalmitis is a severe intraocular infection that, while rare, requires urgent treatment to preserve vision.
According to a 2025 Healio report, patients with diabetes undergoing cataract surgery are 17.4% more likely to develop postoperative endophthalmitis. This makes preoperative risk stratification especially important for diabetic patients. Strict sterile protocols, prophylactic intracameral antibiotics, and careful postoperative monitoring have collectively driven incidence rates to historic lows. For the vast majority of patients, modern surgical hygiene standards make this complication exceedingly unlikely.
How Often Does Cystoid Macular Edema Occur Postoperatively?
Cystoid macular edema occurs postoperatively in approximately 0.82% of routine cataract surgery cases, according to a study published in PMC. CME involves fluid accumulation in the macula that can temporarily reduce central visual acuity.
Anti-inflammatory eye drops prescribed during recovery help prevent this complication. When CME does develop, it typically responds well to topical nonsteroidal anti-inflammatory drugs or corticosteroid therapy. Patients with diabetes or uveitis may face slightly elevated risk, which is why ophthalmologists often tailor postoperative drop regimens for higher-risk individuals.
What Is the Risk of Retinal Detachment After Surgery?
The risk of retinal detachment after cataract surgery is low, generally 0.39%. Retinal detachment occurs when the retina separates from the underlying tissue, and it can develop weeks to months after the procedure.
Certain factors may increase susceptibility, such as high myopia, a history of retinal tears, or complications during surgery like posterior capsule rupture. Prompt recognition of warning signs, including sudden flashes of light, new floaters, or a shadow across the visual field, allows timely intervention. Early surgical repair can often preserve vision when detachment is caught quickly.
How Likely Is Residual Refractive Error After the Procedure?
Residual refractive error after the procedure is possible but increasingly uncommon with modern lens calculation technology. According to a study published by Dove Medical Press, most eyes achieve uncorrected distance visual acuity and corrected distance visual acuity of 20/40 or better with minimal residual refractive error at one month postoperative when using intraoperative aberrometry.
When meaningful refractive error persists, enhancement options are available. LASIK provides better and more predictable outcomes in uncorrected distance visual acuity than PRK for patients requiring correction after cataract surgery. However, patients with prior myopic LASIK or PRK may find IOL power calculations less precise, with fewer than 75% achieving outcomes within ±0.50 D of the intended target.
With ongoing advancements in biometry and surgical guidance, residual refractive surprises continue to decline in frequency and magnitude.
What Does the Cataract Surgery Procedure Feel Like Step by Step?
The cataract surgery procedure feels like a brief, pressure-filled experience with minimal discomfort at each stage. Below, preoperative preparation, intraoperative sensations, and immediate postoperative expectations are covered in detail.
What Happens During Preoperative Preparation on Surgery Day?
Preoperative preparation on surgery day involves a series of steps designed to numb the eye, dilate the pupil, and reduce anxiety before the procedure begins. Upon arrival, the surgical team administers dilating drops to widen the pupil, followed by topical anesthetic drops that numb the eye’s surface. Vital signs are checked, and a mild sedative may be offered through an IV line to help you feel calm.
According to a study published in Acta Scientific Ophthalmology, the most anxiety-provoking preoperative factor for cataract surgery patients is the possibility of surgery failure and loss of the operated eye, with 19.05% of patients citing fear of postoperative pain. Understanding each preparatory step beforehand can significantly ease this anticipatory worry. The entire check-in and preparation process typically takes longer than the surgery itself, often lasting 40 to 60 minutes while the drops take full effect.
What May You Experience During the Procedure Itself?
You may experience mild pressure, light sensitivity, and occasional shifting colors during the procedure itself, but not sharp pain. Once the anesthetic drops have fully numbed the cornea, the surgeon places a small device to keep the eyelids open. Most patients notice a bright light from the operating microscope, which may appear as colorful shapes or a warm glow.
When the phacoemulsification probe breaks apart the cloudy lens using ultrasound energy, a gentle vibrating or buzzing sensation is common. Some patients feel brief moments of dull pressure as the intraocular lens is positioned. The entire surgical portion typically lasts 10 to 15 minutes. Because you remain awake under topical anesthesia, you can hear the surgical team and follow simple instructions, though the sedative keeps most patients relaxed throughout. Any momentary discomfort usually passes within seconds.
What Should You Expect Immediately After Surgery?
You should expect mild grittiness, light sensitivity, and slightly blurred vision immediately after surgery. A protective shield is placed over the treated eye, and the surgical team monitors you briefly in a recovery area. Mild tearing or a watery sensation is normal as the anesthetic wears off over the following hour.
Colors may appear brighter or have a bluish tint as the new intraocular lens transmits light differently than the cloudy natural lens did. Vision typically improves within the first few hours, though some haziness can persist for a day or two. Your ophthalmologist will provide prescribed anti-inflammatory and antibiotic eye drops to use during recovery. Most patients feel well enough to go home within 30–60 minutes of the procedure ending, accompanied by a driver. Knowing what each sensation means helps transform unfamiliar post-surgical feelings into reassuring signs of normal healing.
With the procedural experience understood, choosing the right surgeon and knowing your candidacy factors further builds confidence before surgery day.
Who May Be a Good Candidate for Cataract Surgery?
A good candidate for cataract surgery is typically someone whose vision loss interferes with daily activities and cannot be corrected with glasses alone. The sections below cover when surgery is recommended, which conditions may affect eligibility, and whether patients with diabetes or glaucoma can still qualify.
When Do Ophthalmologists Typically Recommend Cataract Surgery?
Ophthalmologists typically recommend cataract surgery when lens clouding reduces visual acuity enough to impair everyday tasks, such as driving, reading, or working. The key threshold is functional vision loss rather than cataract presence alone.
Most surgeons use a visual acuity benchmark to guide this decision. According to a PMC study published by the National Institutes of Health, cataract extraction should not be recommended for eyes with diabetic retinopathy until visual acuity has deteriorated to 20/40 or worse, as surgery may precipitate vitreous hemorrhage. This 20/40 threshold is widely applied across candidacy evaluations, not just for diabetic patients.
Other factors that may prompt a recommendation include:
- Difficulty with night driving due to glare or halos.
- Inability to perform occupational tasks safely.
- Cataract density interfering with the management of other eye conditions.
In practice, timing the procedure appropriately matters as much as confirming candidacy itself.
What Eye or Health Conditions May Affect Eligibility?
Several eye or health conditions may affect eligibility for cataract surgery. While cataracts alone are straightforward to treat, coexisting ocular or systemic conditions can influence surgical planning, technique selection, and expected outcomes.
Conditions that may complicate candidacy include:
- Diabetic retinopathy: Active proliferative disease may increase the risk of vitreous hemorrhage during or after surgery.
- Glaucoma: Elevated intraocular pressure or prior glaucoma surgery can affect surgical approach and lens implant selection.
- Macular degeneration: Pre-existing retinal damage may limit the visual improvement achievable through cataract removal.
- Corneal disease: Conditions like Fuchs’ dystrophy can affect healing and may require combined procedures.
- Uncontrolled systemic conditions: Poorly managed diabetes or blood-clotting disorders may delay surgical clearance.
None of these conditions automatically disqualify a patient. However, a thorough preoperative evaluation allows the ophthalmologist to weigh risks, adjust technique, and set realistic visual expectations before proceeding.
Can Patients With Diabetes or Glaucoma Still Qualify?
Yes, patients with diabetes or glaucoma can still qualify for cataract surgery in most cases. Both conditions require additional preoperative assessment, but neither represents an absolute contraindication.
For diabetic patients, the ophthalmologist typically evaluates retinal health before scheduling surgery. Stable, well-controlled diabetes with minimal retinopathy generally supports safe candidacy. When dense cataracts are present, femtosecond laser-assisted cataract surgery (FLACS) may offer advantages; according to a study published by Scientific Research Publishing, FLACS is associated with a reduction in effective phacoemulsification time and cumulative dissipated energy compared with conventional phacoemulsification, potentially reducing intraoperative stress on the eye.
For glaucoma patients, surgical planning may involve:
- Adjusting medications to manage intraocular pressure before and after surgery.
- Considering combined cataract and glaucoma procedures when appropriate.
- Selecting IOL types compatible with ongoing glaucoma monitoring.
With proper coordination between the cataract surgeon and any managing specialists, most patients with these conditions can proceed safely and achieve meaningful visual improvement.
What Does Recovery After Cataract Surgery Look Like?
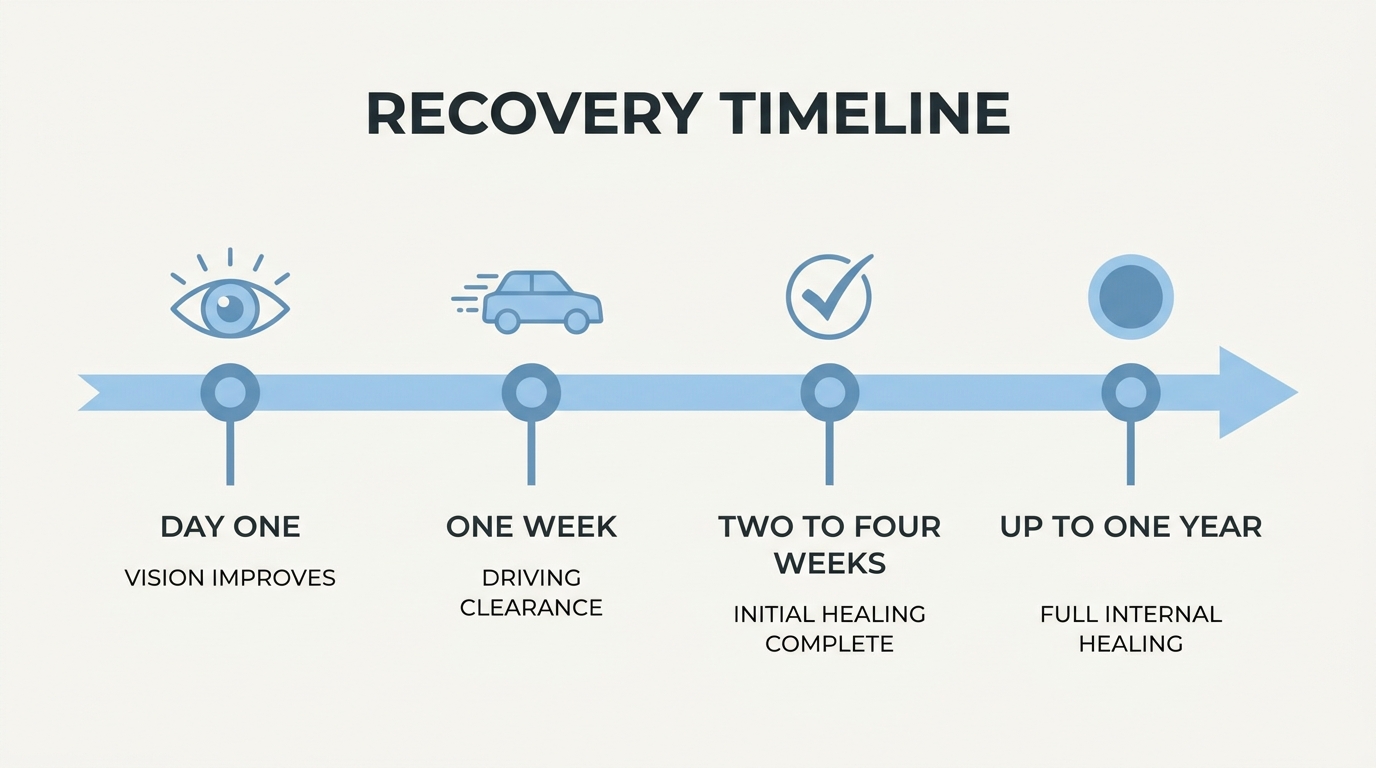
Recovery after cataract surgery generally takes two to four weeks for most patients. The following sections cover initial healing timelines, essential post-operative care instructions, and when you can safely resume driving and daily activities.
How Long Does Initial Healing Typically Take?
Initial healing typically takes two to four weeks after cataract surgery. During this period, the eye gradually stabilizes as inflammation subsides and the incision site closes. Most patients notice improved vision within the first few days, though mild blurriness and light sensitivity are common during early recovery.
While the surface of the eye often heals within the first week or two, complete internal healing takes longer. According to the American Academy of Ophthalmology, it can take up to a year for eyes to feel completely normal after the procedure. This extended timeline reflects the deeper tissue remodeling that continues well beyond the initial recovery window. Patients who understand this distinction tend to set more realistic expectations, which reduces unnecessary concern during follow-up visits.
What Post-Operative Care Instructions Are Most Important?
The most important post-operative care instructions focus on protecting the eye from infection, inflammation, and physical trauma during healing. According to the NHS, post-operative eye drops to help the eye heal and prevent infection are usually required for about four weeks.
Key post-operative care instructions include:
- Use prescribed eye drops on schedule. Anti-inflammatory and antibiotic drops reduce infection risk and control swelling.
- Wear a protective eye shield while sleeping. This prevents accidental rubbing or pressure on the healing eye.
- Avoid rubbing or touching the eye. Even gentle contact can disrupt the incision site.
- Avoid heavy lifting and strenuous activity. Increased eye pressure from straining may compromise the surgical wound.
- Keep water, soap, and dust away from the eye. Contaminants can introduce bacteria during the vulnerable healing period.
Strict adherence to these instructions is one of the most controllable factors in achieving a smooth recovery.
When Can You Resume Driving and Normal Activities?
You can resume driving and normal activities within days to weeks after cataract surgery, depending on how quickly your vision stabilizes. Most patients return to light daily tasks, such as reading and watching television, within one to two days. Driving clearance typically requires a post-operative eye exam confirming adequate visual acuity, which many patients achieve within the first week.
Patients must avoid heavy lifting and vigorous exercise for at least two, as physical strain can increase intraocular pressure during healing. Swimming and hot tubs should also be avoided for several weeks to reduce infection risk. Your ophthalmologist may provide a personalized activity timeline based on your healing progress and any pre-existing conditions.
Understanding recovery milestones helps set practical expectations, and knowing how cataract surgery compares to other vision procedures, such as eyelid surgery, can further inform your decision.
How Does Cataract Surgery Compare to Other Vision Procedures?
Cataract surgery differs from other vision procedures in its purpose, technique, and pain profile. Cataract surgery replaces a diseased natural lens with an intraocular lens (IOL), while refractive procedures like LASIK and PRK reshape the cornea to correct focusing errors. Because cataract surgery treats a progressive medical condition rather than an elective refractive preference, it addresses both visual impairment and the underlying pathology simultaneously.
Pain experience also differs across procedures. Cataract surgery relies on topical and intracameral anesthesia, producing minimal discomfort for most patients during the primary procedure. However, according to a study published in PMC (National Institutes of Health), most patients report higher pain perception in consecutive second-eye cataract surgery compared to the first eye, a nuance rarely discussed with other refractive procedures.
Recovery timelines vary as well. LASIK patients often notice improved vision within hours, while cataract surgery patients typically experience progressive clarity over days to weeks. Yet cataract surgery offers a dual benefit: it simultaneously removes the cataract and corrects refractive error through premium IOL selection, something corneal refractive procedures cannot achieve.
Global access remains another distinguishing factor. Effective cataract surgical coverage stands at 48.2% worldwide in 2025 and is projected to reach 52.3% by 2030, according to the International Agency for the Prevention of Blindness (IAPB). This gap highlights that despite cataract surgery’s strong safety profile, millions still lack access to a procedure that other vision corrections cannot replace.
For patients weighing their options, the key distinction is straightforward: cataract surgery is a medically necessary intervention that restores vision lost to lens opacity, while LASIK and PRK are elective procedures for otherwise healthy eyes. Understanding this difference can help patients approach surgical discussions with their ophthalmologist from a more informed position.
How Can an Education Platform Help You Prepare?
An education platform can help you prepare by providing clinically accurate, easy-to-understand guides. The sections below cover how Eye Surgery Today builds patient confidence and the essential takeaways about cataract surgery safety.
Can Eye Surgery Today’s Guides Help You Feel Confident?
Yes, Eye Surgery Today’s guides can help you feel confident by translating complex surgical concepts into clear, accessible language. Patients who understand what to expect before, during, and after cataract surgery typically experience less preoperative anxiety. Eye Surgery Today addresses this directly through structured educational resources covering IOL selection, step-by-step procedure walkthroughs, and evidence-based safety information. When patients arrive at their consultation already informed, conversations with their surgeon become more productive and focused on personalized care decisions.
For those still in the early research phase, Eye Surgery Today offers free access to “The Insider’s Guide to Cataract Surgery,” designed to answer the most common questions patients have before committing to a procedure.
What Are the Key Takeaways About Why Cataract Surgery Is Pain-Free and Safe in 2026?
The key takeaways about why cataract surgery is pain-free and safe in 2026 are:
- Modern topical and intracameral anesthesia protocols can effectively numb the eye, minimizing discomfort throughout the procedure.
- Femtosecond laser-assisted technology and advanced phacoemulsification systems improve surgical precision while reducing tissue stress.
- Serious complications, such as endophthalmitis and cystoid macular edema, occur at rates well below 1% in routine cases.
- Recovery is typically measured in days to weeks, with most patients resuming normal activities relatively quickly.
According to the American Academy of Ophthalmology, most people can resume normal activities within days or weeks after cataract surgery, though it can take up to a year for the eyes to feel completely normal. This combination of refined pain management, advanced surgical technology, and low complication rates makes cataract surgery one of the most predictable and well-tolerated procedures in modern medicine. Understanding these facts beforehand is the single most effective way to replace fear with confidence.