Immediate Post-Op Instructions: Protecting Your Eye and Healing Well
Immediate post-op instructions for eye surgery are the specific clinical guidelines your surgeon provides to protect the healing eye, prevent complications, and support optimal visual recovery during the critical days and weeks following your procedure.
This guide covers the first 24-hour recovery window and what to expect, physical eye protection strategies, activity and hygiene restrictions, prescribed eye drop protocols, complication warning signs, and nutritional and follow-up care considerations.
The first 24 hours represent the most vulnerable period after eye surgery, as the incision begins closing and the eye’s surface starts to seal. Avoiding movements like bending below the waist during the first 48 hours may help prevent dangerous increases in intraocular pressure that can compromise the fresh surgical site.
Protecting the eye requires consistent use of a rigid eye shield (especially during sleep), wraparound UV sunglasses outdoors, and deliberate habits to prevent rubbing or touching the operative site. Activity restrictions include avoiding heavy lifting, swimming for at least two weeks, and driving until your surgeon confirms adequate visual acuity.
Prescribed eye drops play a central role in preventing infection and controlling inflammation. Proper sequencing, sterile administration technique, and consistent scheduling all influence healing outcomes.
Recognizing warning signs is equally important. Symptoms like rapidly worsening pain, sudden vision loss, heavy discharge, or redness that intensifies after the first few days may indicate serious complications requiring emergency evaluation.
Follow-up appointments, typically scheduled within 24 to 48 hours for the first visit, allow your ophthalmologist to measure eye pressure, assess healing, and catch treatable issues early. Targeted nutrition, including vitamins C and E, carotenoids, and amino acids, may further support tissue repair during recovery.
Why Are the First 24 Hours After Eye Surgery So Critical?
The first 24 hours after eye surgery are critical because the surgical incision begins closing and the eye’s surface starts to seal, making this window the most vulnerable period for complications. Below, the key healing processes and precautions during this timeframe are explained.
During this initial recovery phase, the small incision created during the procedure starts to close while the outer surface of the eye seals shut. According to the American Academy of Ophthalmology, although surface closure begins within the first day, the smooth barrier underneath the eye’s surface can take several additional weeks to fully heal. This gap between surface sealing and deeper tissue recovery is precisely what makes early post-op behavior so consequential.
Because the eye remains structurally fragile during this window, even minor physical actions can disrupt the healing process. Patients should avoid bending over or placing their head below waist level during the first 48 hours, as these positions can increase intraocular pressure and strain the fresh incision site. Gentle movements, upright positioning, and strict adherence to prescribed eye drop schedules all help protect the delicate tissue as it begins to stabilize.
For most patients, this period sets the foundation for the weeks of recovery that follow. Understanding what to expect during these early hours can help reduce anxiety and prevent avoidable setbacks.
What Should You Expect Immediately After Eye Surgery?
Immediately after eye surgery, you can expect temporary blurriness, mild discomfort, and light sensitivity. Most patients heal completely within 8 weeks. The sections below cover normal vision changes, common sensations, and how long you will stay at the surgery center.
What Vision Changes Are Normal Right After Surgery?
Normal vision changes right after surgery include blurriness, mild redness, and increased light sensitivity. These typically improve within the first few days as the eye begins healing.
According to the National Eye Institute, about 9 out of 10 people who undergo cataract surgery experience improved vision afterward, although vision may initially be blurry during the recovery period. Redness in the white of the eye is also expected because the procedure temporarily damages small blood vessels, a change that usually resolves within a few days.
While early blurriness can feel concerning, it is a standard part of the healing process and not necessarily a sign of complications. However, certain symptoms require immediate attention:
- Rapidly progressive pain or worsening vision between days 3 and 5 post-op
- Sudden increase in floaters, flashes of light, or small dark spots
- Heavy ocular discharge combined with a very red eye
These warning signs may indicate acute postoperative endophthalmitis, a rare but serious infection. Contact your eye doctor immediately if any of them develop.
What Sensations Like Pain or Itching Are Common Post-Op?
Sensations like pain or itching that are common post-op include scratchiness, a gritty feeling, mild stinging, and light pressure around the eye. Most of these resolve gradually as the eye heals.
According to the American Academy of Ophthalmology, scratchiness or a feeling that something is in the eye is common after cataract surgery, though this sensation may persist longer in patients with dry eye or other ocular surface diseases. Mild itching often accompanies healing as well, particularly in the first 48 hours.
Gentle tearing and occasional dull aching are also within the normal range. However, persistent severe pain, throbbing that worsens over time, or sharp stabbing sensations are not typical and should prompt an immediate call to your surgeon. Resisting the urge to rub or touch the eye is essential, since rubbing can disrupt healing and increase infection risk.
How Long Will You Stay at the Surgery Center Before Going Home?
You will typically stay at the surgery center for 30 to 60 minutes after eye surgery before going home. This brief observation period allows the surgical team to monitor your initial recovery, check for any immediate complications, and confirm that your eye pressure remains stable.
During this time, a staff member will review your post-operative care instructions, including your eye drop schedule and activity restrictions. Because your vision will still be blurry and your eye may be sensitive, you cannot drive yourself home. Arranging a ride in advance is essential.
Most patients feel well enough to leave comfortably within the hour, making eye surgery one of the more streamlined outpatient procedures. With discharge instructions in hand, the next priority is understanding how to physically protect the eye during recovery.
How Should You Protect Your Eye After Surgery?
You should protect your eye after surgery by wearing a rigid eye shield, avoiding contact with the eye, and using protective eyewear outdoors. The following subsections cover shield use, sleep precautions, touch prevention, and outdoor eye protection.
How Should You Wear and Care for Your Eye Shield?
You should wear and care for your eye shield by positioning it securely over the operated eye and keeping it clean between uses. The shield is a rigid, transparent or perforated guard that sits over the eye socket without pressing directly on the eyeball. Your surgical team will typically tape it in place before you leave the surgery center.
To care for the shield properly:
- Clean it daily with mild soap and warm water, then air dry before reapplying.
- Use medical tape to secure the shield firmly to the brow and cheekbone area.
- Avoid touching the inside surface that faces your eye.
- Replace tape strips each time you reattach the shield to maintain a secure hold.
According to the NHS, patients should avoid rubbing the eye and take precautions to keep it protected throughout the early recovery period. A well-maintained shield is the single most effective barrier against accidental bumps and pressure during the critical first days of healing.

When Should You Wear Your Eye Shield During Sleep?
You should wear your eye shield during sleep for at least the first week after surgery, or as long as your surgeon recommends. Sleep is the highest-risk period for accidental eye contact because you cannot consciously control your hand movements. Many patients unknowingly rub or press against their face while sleeping, which can disrupt the healing incision.
Wearing the shield at night serves two purposes:
- It prevents direct pressure from pillows, hands, or bedding against the operated eye.
- It acts as a physical reminder if your hand drifts toward your face during sleep.
Some surgeons extend the recommendation to two weeks for patients who are restless sleepers. Taping the shield securely before bed, rather than simply placing it loosely, reduces the chance of it shifting overnight. Consistent nightly use during this window helps the surgical site heal without mechanical interference.
How Can You Avoid Accidentally Rubbing or Touching Your Eye?
You can avoid accidentally rubbing or touching your eye by building conscious habits and using physical barriers during the recovery period. The urge to rub may feel strong, especially when mild itching or a foreign-body sensation occurs. As the American Academy of Ophthalmology notes, scratchiness and a feeling that something is in the eye are common after cataract surgery, and these sensations should gradually subside as healing progresses.
Practical strategies to prevent accidental contact include:
- Keeping your hands occupied or folded in your lap when the urge arises.
- Using prescribed lubricating drops to relieve itching rather than rubbing.
- Wearing your eye shield during naps and sleep when unconscious rubbing is most likely.
- Placing visual reminders near mirrors and bedside tables during the first week.
Resisting the impulse to rub, even gently, is one of the most important habits to maintain throughout early recovery.
What Protective Eyewear Should You Use Outdoors?
The protective eyewear you should use outdoors after eye surgery includes wraparound sunglasses with full UV protection. The healing eye is highly sensitive to bright light, wind, and airborne debris during the first several weeks of recovery. Standard sunglasses may leave gaps at the sides where dust or wind can reach the eye.
Wraparound frames offer several advantages:
- They block UV rays from multiple angles, reducing light sensitivity and protecting the retina.
- They shield against wind, pollen, and small particles that could irritate the surgical site.
- They serve as a physical barrier, discouraging accidental touching in public settings.
For the best protection, choose lenses rated UV 400 or higher. On overcast days, wearing them remains important because UV exposure persists even without direct sunlight. Keeping protective eyewear on whenever you step outside during recovery is a simple habit that significantly lowers the risk of irritation or injury.
With your eye properly shielded and protected, understanding which daily activities to modify next helps support a smooth recovery timeline.
What Activities Should You Avoid During Eye Surgery Recovery?
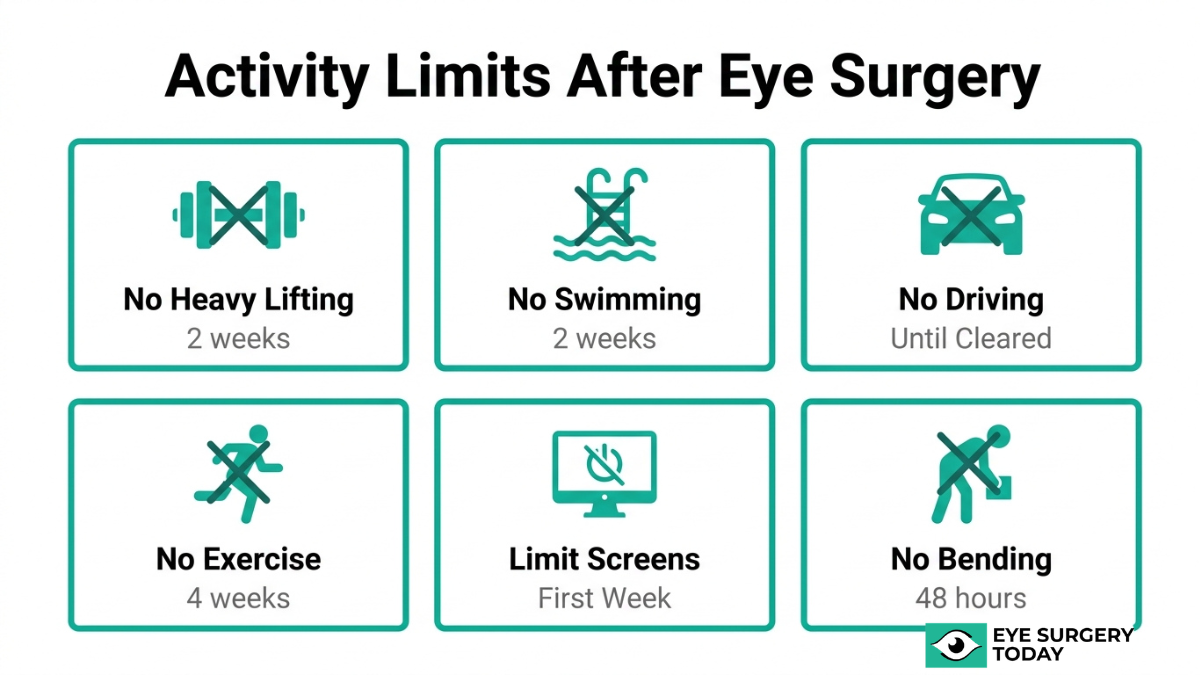
Activities you should avoid during eye surgery recovery include heavy lifting, bending, strenuous exercise, driving, swimming, and prolonged screen time. The sections below cover specific timelines for each restriction.
What Lifting and Bending Restrictions Apply After Surgery?
Lifting and bending restrictions after surgery focus on preventing dangerous increases in eye pressure during the critical early healing window. Bending over or positioning the head below the waist should be avoided for at least 48 hours after the procedure, as these movements can elevate intraocular pressure and stress the healing incision.
General guidelines for lifting and bending include:
- Avoid lifting anything heavier than 10 to 15 pounds for the first one to two weeks.
- Do not bend at the waist to pick up objects; squat with knees bent instead.
- Skip household chores that require stooping, such as mopping or gardening.
- Avoid straining during bowel movements, as this also raises eye pressure.
These restrictions may seem minor, but even brief spikes in intraocular pressure can compromise surgical outcomes during the first week. Your eye surgeon can provide personalized guidance on when to resume normal activity levels.
When Is It Safe to Resume Exercise After Eye Surgery?
Exercise is generally safe to resume in gradual stages after eye surgery, starting with light activity. According to the American Academy of Ophthalmology, patients should follow a phased return to physical activity based on how the eye heals.
A typical exercise timeline looks like this:
- Days 1 to 3: Light walking at a comfortable pace is usually acceptable.
- Week 1: Gentle stretching and slow-paced activities may be introduced if approved by your surgeon.
- Weeks 2 to 4: Moderate activities, such as stationary cycling or light jogging, can often resume.
- After 4 weeks: Contact sports, heavy weightlifting, and high-impact activities may be cleared following a post-operative evaluation.
Rushing back into intense exercise remains one of the most common recovery mistakes. Waiting for explicit clearance from your eye care provider before any vigorous activity protects both the incision site and long-term visual outcomes.
Can You Drive After Eye Surgery and When?
You can drive after eye surgery once your vision has stabilized enough to meet legal driving standards, which varies by procedure and individual healing. Most patients should avoid driving for at least 24 hours after surgery, and many surgeons recommend waiting until the first follow-up appointment confirms adequate visual acuity.
Key factors that determine when driving is safe include:
- Visual clarity in the operated eye, particularly the ability to read road signs.
- Absence of significant blurriness, light sensitivity, or depth perception issues.
- Discontinued use of sedating pain medications that may impair reaction time.
- Surgeon clearance, typically given at the first or second post-operative visit.
Driving too soon puts both the patient and others at risk. Even if vision feels adequate, depth perception and contrast sensitivity can remain subtly impaired for several days following surgery.
How Long Should You Avoid Swimming and Hot Tubs?
You should avoid swimming and hot tubs for at least two weeks after eye surgery. According to the American Academy of Ophthalmology, swimming and exposing the eye to water should be avoided during this period to prevent infection or irritation.
Bodies of water, including pools, lakes, oceans, and hot tubs, harbor bacteria and chemical irritants that can penetrate a healing surgical incision. Chlorine alone does not eliminate infection risk. Even wearing goggles is insufficient protection, since water can still seep around the seal and contact the eye.
Some surgeons extend this restriction to four weeks depending on the procedure and healing progress. Showers are generally permitted earlier with precautions, but submerging the face or allowing direct water contact with the eye should be strictly avoided until cleared.
When Can You Safely Return to Screen Time and Reading?
You can safely return to screen time and reading in short intervals within the first 24 to 48 hours for most patients, though moderation is essential. Eyes may tire quickly after surgery, so brief sessions of 15 to 20 minutes with frequent breaks help prevent strain.
Practical tips for comfortable screen use during recovery include:
- Follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds.
- Reduce screen brightness and increase font size to minimize eye fatigue.
- Use preservative-free artificial tears to combat dryness from reduced blinking.
- Avoid reading in dim lighting, which forces the eye to work harder.
Unlike swimming or heavy lifting, screen time is less about infection risk and more about comfort. Most patients find that screen tolerance improves steadily throughout the first week, with near-normal use possible within two weeks.
With activity restrictions understood, proper use of prescribed eye drops plays an equally important role in protecting your surgical results.
How Should You Use Your Prescribed Eye Drops After Surgery?
You should use your prescribed eye drops after surgery by following your surgeon’s specific schedule, applying them in the correct order, and maintaining strict hygiene to prevent contamination. The sections below cover drop sequencing, proper administration technique, and what to do if you miss a dose.
What Is the Correct Order for Applying Multiple Eye Drops?
The correct order for applying multiple eye drops is typically determined by your surgeon’s instructions, which may vary based on the specific medications prescribed. Most post-op regimens include an antibiotic drop, an anti-inflammatory drop, and sometimes a steroid or lubricating drop.
General sequencing guidelines include:
- Administer thinner, water-based drops before thicker, gel-based drops so the thinner solution can absorb first.
- Wait at least 5 minutes between different eye drop medications to prevent one drop from washing out another.
- Apply lubricating drops or artificial tears last, as their viscosity can create a barrier that slows absorption of medicated drops.
- Follow any numbered schedule your surgeon provides, since certain medications may need more frequent daily dosing than others.
If your regimen feels confusing, write out a simple chart with drop names and times. Consistency matters more than perfection, and a written schedule reduces the chance of skipping a medication entirely.
How Do You Properly Administer Eye Drops Without Contamination?
You properly administer eye drops without contamination by keeping the dropper tip away from your eye, hands, and any surface. Even brief contact can introduce bacteria, which poses a serious risk during the vulnerable post-operative healing window.
Follow these steps for clean application:
- Wash your hands thoroughly with soap and water before handling the bottle.
- Tilt your head back or lie down, and gently pull your lower eyelid down to create a small pocket.
- Hold the dropper approximately one inch above the eye and squeeze one drop into the lower eyelid pocket.
- Close your eye gently for 1 to 2 minutes and press lightly on the inner corner near the nose to reduce drainage into the tear duct.
- Avoid blinking rapidly, as this can push the drop out before absorption.
- Replace the cap immediately without touching the tip.
Proper technique helps each dose reach the eye’s surface effectively, supporting both infection prevention and healing.
What Happens If You Miss a Dose of Post-Op Eye Drops?
Missing a dose of post-op eye drops is generally not cause for alarm if handled promptly. According to Eagle Eye Care, patients who accidentally miss a postoperative eye drop dose are advised to administer the missed dose as soon as they remember, but they should avoid doubling up if it is nearly time for the next scheduled dose.
Key points to keep in mind:
- A single missed dose is unlikely to derail recovery, but repeated missed doses can increase the risk of inflammation or infection.
- If you realize you missed a dose close to your next scheduled time, skip the missed dose and resume your normal schedule.
- Never apply two doses at once to compensate, as overdosing can irritate the eye or disrupt the medication’s intended effect.
- Contact your surgeon’s office if you miss multiple doses in a row, so they can advise whether any adjustment is needed.
Staying consistent with your drop schedule is one of the simplest ways to protect your surgical outcome. With proper hygiene habits in place, daily routines like bathing also require careful adjustments during recovery.
How Should You Handle Hygiene and Bathing After Eye Surgery?
You should handle hygiene and bathing after eye surgery by keeping water, soap, and cosmetics away from the healing eye. The sections below cover safe showering techniques, when normal face washing can resume, and makeup timelines.
How Can You Shower Safely Without Getting Water in Your Eye?
You can shower safely without getting water in your eye by angling your head so the stream hits the back of your skull and flows away from your face. Keeping your operated eye closed throughout adds a second layer of protection. According to the NHS, patients should avoid getting water in the eye following cataract surgery, as exposure can introduce bacteria to the healing incision site.
Practical steps for a safe post-op shower include:
- Tilting your head backward or turning away from the showerhead so water runs down the back of your neck.
- Keeping the water pressure low to reduce splashing.
- Avoiding hair washing for the first 24 to 48 hours; when you do resume, lean your head back rather than forward.
- Patting the area around the eye dry with a clean towel instead of rubbing.
A lukewarm temperature is gentler on the body and less likely to produce steam that settles on the eye’s surface. For most patients, these precautions remain important for at least the first one to two weeks, until the surgeon confirms the incision has sealed adequately.
When Is It Safe to Wash Your Face Normally Again?
It is generally safe to wash your face normally again once your surgeon confirms the eye’s surface has healed sufficiently, which typically occurs around one to two weeks after surgery. During the first 24 hours, the small incision begins to close and the surface of the eye seals shut, yet as the American Academy of Ophthalmology notes, the smooth barrier underneath can take several additional weeks to fully heal.
Until clearance is given, a safer approach involves:
- Using a damp washcloth to gently wipe the forehead, cheeks, and chin while avoiding the eye area entirely.
- Cleaning around the eye only with a sterile saline pad or a cotton ball lightly moistened with cooled boiled water.
- Skipping facial cleansers, scrubs, or exfoliants near the operative site.
Resuming a full face-washing routine too early can force contaminated water into the still-healing incision, raising infection risk. Even after the two-week mark, gentle technique and mild products are advisable until the follow-up appointment confirms complete surface recovery.
Can You Wear Makeup After Eye Surgery and When?
You can wear makeup after eye surgery, but not immediately. Most surgeons recommend avoiding all eye makeup for at least one to two weeks following the procedure. According to the NHS, patients are specifically advised not to wear eye makeup during the initial recovery period after cataract surgery.
Key guidelines for returning to cosmetics include:
- Waiting at least one week before applying products to the face away from the eye, such as foundation on the cheeks or lipstick.
- Waiting a minimum of two weeks, or until your surgeon gives clearance, before applying mascara, eyeliner, or eyeshadow.
- Discarding old eye makeup and opening fresh products to minimize bacterial contamination.
- Avoiding waterproof formulas initially, because the aggressive removers they require can irritate healing tissue.
Makeup particles are a common and often underestimated source of post-surgical contamination. Even a tiny flake of mascara or eyeshadow pigment can introduce bacteria beneath the eyelid and compromise the incision site. Patience with cosmetics during recovery is one of the simplest ways to protect your surgical outcome.
With hygiene habits in place, recognizing warning signs of complications becomes the next priority.
What Are the Possible Risks and Complications to Watch For?
The possible risks and complications to watch for after eye surgery include signs of infection, sudden vision loss, increased eye pressure, and abnormal redness or swelling.
What Signs of Infection Should Prompt an Emergency Call?
Signs of infection that should prompt an emergency call include rapidly worsening pain, increasing redness, eye discharge, and declining vision. Acute postoperative endophthalmitis, the most serious infection after eye surgery, generally presents within one to two weeks, most frequently between days three and five. According to EyeWiki (American Academy of Ophthalmology), 94.3% of patients with acute endophthalmitis reported blurred vision, 82.1% reported red eye, and 74% reported pain.
Because over 25% of endophthalmitis cases present without pain, vision changes and discharge alone can signal a serious problem. Key warning signs include:
- A white or yellowish collection of fluid visible inside the eye (hypopyon)
- Lid swelling that worsens rather than improves
- Thick or increasing eye discharge
- Vision that deteriorates rapidly after an initial period of improvement
High-risk and functionally monocular patients should be seen within 24 hours of surgery, while routine patients should typically be seen within 48 hours. If any of these signs appear before a scheduled follow-up, contact your eye surgeon’s office immediately rather than waiting.
When Does Sudden Vision Loss Indicate a Serious Problem?
Sudden vision loss indicates a serious problem when it occurs after an initial period of stable or improving sight. A gradual clearing of blurriness over the first few days is expected; however, sharp, unexplained drops in vision after that early window may suggest complications such as endophthalmitis, retinal detachment, or significant inflammation.
Symptoms that warrant urgent evaluation include:
- A sudden curtain or shadow moving across your field of vision
- New flashes of light or a sudden increase in floaters
- Complete loss of vision in the operated eye
- Vision that worsens dramatically within hours rather than days
Any of these changes require same-day contact with your surgeon. Delaying evaluation when vision deteriorates rapidly can reduce the effectiveness of treatment, so treating sudden vision loss as a medical emergency is always the safest approach.
How Do You Recognize Increased Eye Pressure After Surgery?
You recognize increased eye pressure after surgery by monitoring for a deep, aching pain around or behind the eye, nausea, headache, and a noticeable worsening of blurry vision. Unlike surface irritation or mild scratchiness, pressure-related discomfort tends to feel like intense internal pressure rather than external soreness.
According to Cataract & Refractive Surgery Today, intraocular pressure peaks most commonly occur 8 to 12 hours after the procedure, with only 1.3% to 10% of cases recording an IOP higher than 30 mm Hg at 24 hours postoperatively. Symptoms to watch for include:
- A dull, throbbing ache that does not improve with prescribed pain medication
- Seeing halos or rainbow-colored rings around lights
- Sudden onset of nausea without another obvious cause
Most mild pressure spikes resolve on their own or respond quickly to medication. However, persistent or severe symptoms within the first 24 hours should be reported to your surgical team promptly, as untreated elevated IOP can compromise surgical outcomes.
What Level of Redness or Swelling Is Abnormal Post-Op?
The level of redness or swelling that is abnormal post-op is any that intensifies or spreads after the first few days rather than gradually improving. Some redness in the white of the eye is normal immediately after surgery because the procedure temporarily disrupts small surface blood vessels, and mild lid puffiness is expected during the first 48 hours.
Redness and swelling become concerning when they show these patterns:
- Redness that deepens in color or expands beyond the initial area after day two or three
- Swelling that worsens progressively instead of subsiding
- Redness accompanied by thick discharge, increasing pain, or declining vision
- The entire eye appearing uniformly deep red rather than showing patchy, localized irritation
Normal post-surgical redness typically fades within a few days. In clinical practice, the trajectory of symptoms matters more than the symptoms themselves. Redness that steadily improves, even if initially dramatic, is far less concerning than mild redness that reverses course and worsens. When in doubt, contacting your surgeon early is always preferable to waiting.
With potential complications understood, knowing when to attend follow-up appointments helps catch issues early.
What Should You Know About Follow-Up Appointments After Surgery?
Follow-up appointments after surgery allow your eye doctor to monitor healing, measure eye pressure, and catch complications early. These visits typically follow a structured schedule based on your risk level and recovery progress.
Your ophthalmologist may schedule the first postoperative visit within 24 to 48 hours, depending on your individual risk factors. According to the American Academy of Ophthalmology’s clinical benchmarks, functionally monocular and high-risk patients should be seen within 24 hours of cataract surgery, while routine patients should typically be seen within 48 hours.
A standard postoperative eye exam includes several key components:
- Interval history to assess how symptoms have changed since surgery.
- Measurement of visual function and intraocular pressure (IOP).
- Slit-lamp biomicroscopy to examine the eye’s structures under magnification.
- Patient counseling on medications, activity restrictions, and warning signs.
The frequency and timing of subsequent visits depend on factors such as incision size and configuration, whether sutures need removal, and the overall medical condition of the eye. Some patients require weekly check-ins during the first month, while others with uncomplicated recoveries may space visits further apart.
Missing or skipping follow-up appointments can delay the detection of treatable issues like elevated IOP or early signs of infection. Even when recovery feels smooth, these evaluations provide objective data that symptoms alone cannot reveal. Consistent follow-through with your prescribed visit schedule is one of the most straightforward steps you can take to protect your surgical outcome and ensure ongoing eye wellness. With your follow-up plan established, the right nutrition and medication choices can further support the healing process.

What Foods and Medications May Help or Hinder Eye Healing?
Foods and medications that may help or hinder eye healing include nutrient-rich foods that support tissue repair and certain drugs that can interfere with recovery. The subsections below cover beneficial nutrients, medications to discuss with your surgeon, and supplements that may aid healing.
Which Nutrients Support Faster Eye Recovery?
Nutrients that support faster eye recovery include vitamins C and E, carotenoids, and amino acids. Vitamin C contributes to collagen formation, which is essential for tissue repair in the cornea and surrounding structures. Vitamin E acts as an antioxidant that may help protect healing cells from oxidative stress.
According to a National Institutes of Health review, results from the Age-Related Eye Disease Study (AREDS) I and II indicate that supplementation with vitamins C and E, along with carotenoids, can decrease the risk of macular degeneration development and may support overall ocular health during recovery.
Foods rich in these nutrients include:
- Citrus fruits, bell peppers, and strawberries for vitamin C.
- Nuts, seeds, and leafy greens for vitamin E.
- Carrots, sweet potatoes, and spinach for carotenoids such as lutein and zeaxanthin.
- Lean proteins, eggs, and legumes for amino acids that support epithelial healing.
Staying well hydrated also helps maintain tear film quality, which can reduce dry eye discomfort during recovery.
What Medications Should You Discuss with Your Surgeon Before Recovery?
Medications you should discuss with your surgeon before recovery include blood thinners, anti-inflammatory drugs, and any prescription eye drops unrelated to your procedure. Blood-thinning medications such as warfarin or aspirin may increase the risk of intraocular bleeding, so your surgeon needs to weigh the risks of pausing them against cardiovascular concerns.
Over-the-counter anti-inflammatory drugs like ibuprofen can sometimes interfere with prescribed post-operative eye drops. Corticosteroid or immunosuppressive medications may also alter healing timelines. Because every patient’s medication profile differs, providing your full medication list before surgery allows your care team to adjust dosing schedules safely.
If a postoperative eye drop dose is accidentally missed, administer it as soon as you remember, but avoid doubling up if the next scheduled dose is near. Never discontinue or modify any medication without your surgeon’s guidance.
Can Supplements Like Omega-3s or Vitamin C Aid Eye Healing?
Yes, supplements like omega-3s and vitamin C can aid eye healing by supporting anti-inflammatory pathways and tissue repair. Omega-3 fatty acids, commonly found in fish oil, may help improve tear production and reduce ocular surface inflammation during recovery. Vitamin C plays a direct role in collagen synthesis, which is critical for corneal wound closure.
According to a study published through the National Institutes of Health, oral supplementation with amino acids has been shown to significantly improve corneal nerve restoration and epithelial healing after photorefractive keratectomy, especially within the first 3 days post-surgery. This suggests that targeted nutritional support during the earliest recovery window can meaningfully influence outcomes.
However, not all supplements are safe to take alongside post-operative medications. High-dose vitamin E, for example, may thin the blood and increase bleeding risk. Always confirm supplement use with your eye surgeon before starting anything new during recovery.
With nutrition and medication considerations addressed, surgeon-reviewed resources can help guide the rest of your post-op journey.
How Can Surgeon-Reviewed Resources Help You Navigate Post-Op Recovery?
Surgeon-reviewed resources can help you navigate post-op recovery by providing clinically accurate, easy-to-understand guidance at every stage of healing. The sections below cover how Eye Surgery Today supports your journey and the key takeaways from this guide.
Can Eye Surgery Today’s Expert Guides Support Your Healing Journey?
Yes, Eye Surgery Today’s expert guides can support your healing journey by translating complex surgical recovery protocols into clear, actionable steps. Every resource on the platform is surgeon-reviewed, ensuring clinical accuracy without overwhelming medical jargon.
Eye Surgery Today covers the full scope of post-op care, including:
- Detailed first-24-hour recovery timelines and what to expect.
- Eye drop schedules and proper administration techniques.
- Activity restriction guides for exercise, driving, and bathing.
- Warning sign checklists for infections, pressure spikes, and vision changes.
- Follow-up appointment preparation and what your surgeon will evaluate.
For patients navigating cataract surgery or refractive procedures, having a single trusted source reduces confusion and supports better adherence to post-operative instructions. Eye Surgery Today was built to bridge the gap between a brief clinical visit and the questions that arise once you are home recovering.
What Are the Key Takeaways About Immediate Post-Op Eye Care We Covered?
The key takeaways about immediate post-op eye care covered in this guide center on protection, compliance, and vigilance during the critical healing window.
- Protect the eye physically. Wear your eye shield as directed, especially during sleep, and avoid rubbing or touching the surgical eye.
- Follow activity restrictions carefully. Avoid heavy lifting, bending below the waist, swimming, and driving until your surgeon clears you.
- Use prescribed eye drops on schedule. Apply drops in the correct order, maintain sterile technique, and never double up on missed doses.
- Maintain safe hygiene practices. Keep water, soap, and makeup away from the eye during early recovery.
- Know the warning signs. Sudden vision loss, rapidly increasing pain, excessive redness, or discharge warrant an immediate call to your surgeon.
- Attend every follow-up appointment. These visits assess healing, measure intraocular pressure, and catch complications early.
According to Navigate Patient, competitor content gaps in ophthalmology patient education often include the lack of standardized processes for repeated messaging and educational videos to reinforce post-operative instructions. Eye Surgery Today addresses this gap with structured, surgeon-reviewed guides designed for ongoing reference throughout recovery.