Vision After Cataract Surgery: What to Expect
Vision after cataract surgery refers to the gradual visual improvement that occurs as the eye heals and adapts to a new intraocular lens (IOL) following removal of the clouded natural lens.
This guide covers immediate post-surgical vision changes, the week-by-week recovery timeline, common visual symptoms during healing, how IOL selection shapes long-term clarity, potential complications that may affect results, and steps you can take to support the best possible outcome.
Immediately after surgery, most patients notice brighter light and more vivid colors, though haziness from corneal swelling, inflammation, and tear film instability is normal. These effects typically begin improving within 24 to 48 hours.
The broader recovery timeline spans several weeks. Vision often sharpens meaningfully during the first week, with many patients resuming driving within one to two weeks. Full stabilization of the visual prescription may take four to eight weeks as the IOL settles and residual swelling resolves.
Temporary symptoms such as halos, glare, dry eye, floaters, and intensified color perception are common during healing and generally diminish as the eye adjusts. Recognizing these as expected parts of recovery can help reduce unnecessary concern.
IOL type directly influences post-surgical clarity and glasses dependence. Monofocal lenses may deliver strong distance vision with preserved contrast sensitivity, while multifocal and extended depth of focus designs can reduce reliance on glasses across multiple distances, sometimes with mild optical trade-offs.
Pre-existing conditions such as macular degeneration, glaucoma, or diabetic eye disease can place limits on achievable visual outcomes, even when surgery itself is successful. Complications like posterior capsule opacification or cystoid macular edema, while treatable, also require awareness for early detection.
Following post-operative medication schedules, protecting the eye during early healing, and attending all follow-up appointments remain among the most reliable ways to safeguard long-term visual results.
How Does Vision Change Immediately After Cataract Surgery?
Vision changes immediately after cataract surgery due to normal postoperative inflammation, mild corneal swelling, and a temporarily unstable tear film. The sections below cover first-day expectations, causes of early blurriness, and the typical clearing timeline.
What Does Vision Look Like on the First Day After Surgery?
Vision on the first day after surgery typically appears hazy, washed out, or slightly foggy. Most patients notice an immediate improvement in brightness compared to pre-surgery vision, even though clarity has not yet fully developed. Colors may seem more vivid because the yellowed cataract lens has been replaced with a clear intraocular lens (IOL).
Some patients also experience mild light sensitivity during the first 24 hours. Clinical guidelines recommend that the initial postoperative examination should typically occur within 24 hours to monitor for intraocular pressure spikes and early complications, according to a report published by the American Academy of Ophthalmology via PMC. Fluctuations in sharpness throughout the day are common and not a cause for concern at this stage.
The degree of visual improvement on day one varies depending on factors such as pre-existing eye conditions, the type of IOL implanted, and individual healing response. Even with noticeable haziness, most patients can see well enough to move around safely at home.
Why Is Vision Blurry Right After Cataract Surgery?
Vision is blurry right after cataract surgery primarily because of three interrelated factors: postoperative inflammation, corneal edema, and tear film instability. During phacoemulsification, the ultrasound energy used to break apart the clouded lens can cause mild swelling in the corneal tissue, a condition known as striate keratopathy. This swelling temporarily distorts how light passes through to the retina.
Inflammation inside the eye is a natural healing response. While controlled with prescribed anti-inflammatory drops, it takes several days to subside enough for vision to sharpen. The tear film, disrupted by the surgical incision and exposure during the procedure, also needs time to restabilize; until it does, visual quality may fluctuate.
Serious causes of persistent blurriness are rare. According to the American Academy of Ophthalmology, the overall incidence rate of acute-onset endophthalmitis after cataract surgery is approximately 0.04% to 0.2%. In most cases, early blurriness resolves predictably as the eye heals and inflammation decreases.
How Long Does It Take for Vision to Clear After Surgery?
Vision typically takes one to four weeks to clear substantially after cataract surgery, though the exact timeline varies by individual. Many patients notice meaningful improvement within the first few days, with sharpness continuing to develop gradually.
According to clinical data from The Vision Institute, vision typically begins to improve within the first week post-surgery, with many patients resuming driving within one to two weeks once vision has stabilized and been cleared by a surgeon. Full stabilization of the visual prescription, however, may take four to six weeks as residual corneal swelling resolves and the IOL settles into its final position.
Patients with pre-existing conditions, such as high myopia or diabetic eye disease, may experience a somewhat longer clearing period. In practice, the first week tends to bring the most dramatic improvement, while the remaining weeks involve subtler refinements in contrast and focus. If blurriness worsens rather than improves after the first few days, contacting the surgical team promptly is important.
Understanding immediate recovery sets the stage for what comes next in the broader vision recovery timeline.
What Does the Vision Recovery Timeline Look Like After Cataract Surgery?
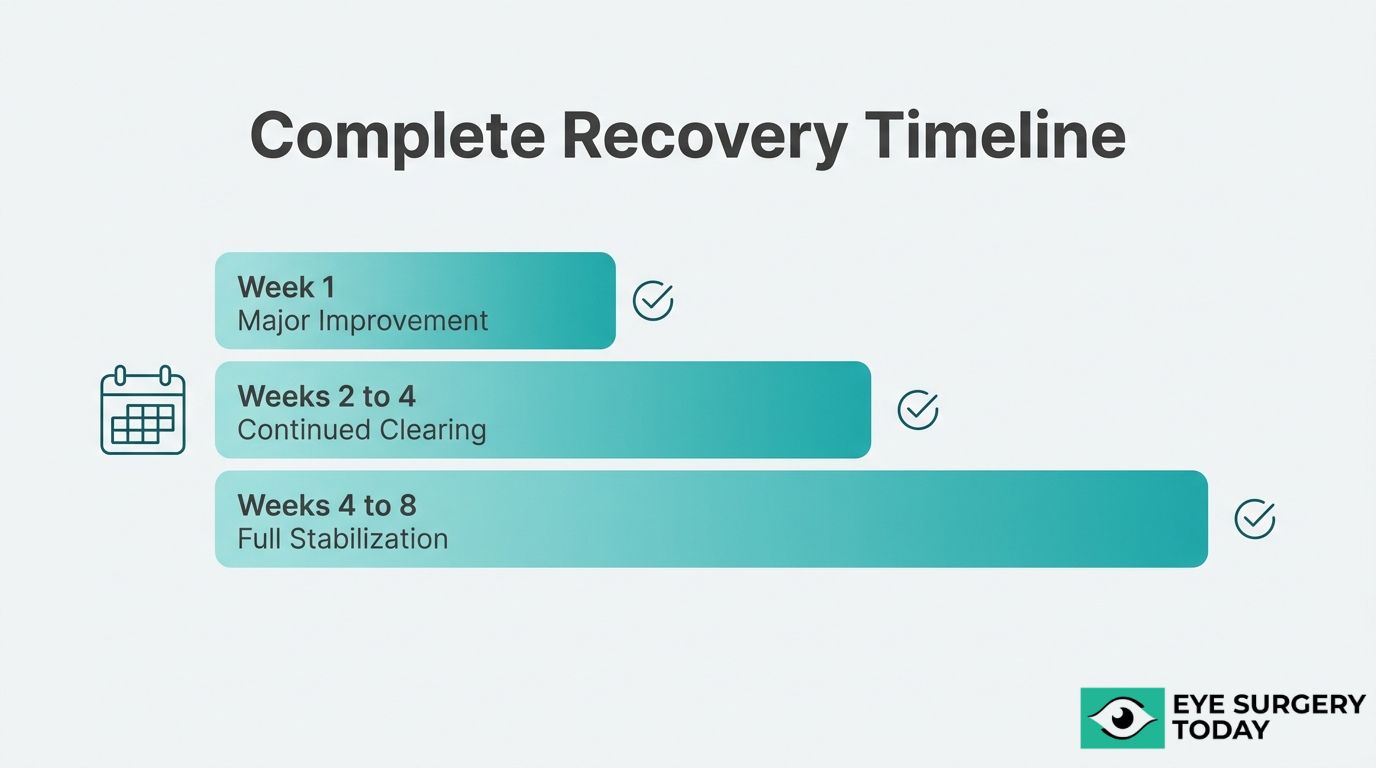
The vision recovery timeline after cataract surgery spans several weeks, with noticeable improvement beginning in the first few days. The sections below cover what to expect during the first week, weeks one through four, and when vision fully stabilizes.
What Can You Expect During the First Week of Recovery?
During the first week of recovery, you can expect gradual clearing of vision alongside some residual blurriness. Most patients notice improved clarity within the first 24 to 48 hours, though mild haziness is common during this early phase.
Several factors contribute to this initial blurriness:
- Postoperative inflammation inside the eye needs time to resolve.
- Mild corneal swelling may temporarily distort light entering the eye.
- The tear film can remain unstable for several days after the procedure.
Clinical guidelines recommend that the initial postoperative examination occur within 24 hours to monitor for intraocular pressure spikes and early complications, according to a recommendation referenced by the American Academy of Ophthalmology. Prescribed eye drops, including anti-inflammatory and antibiotic formulations, play a critical role during this window. Patients who follow their medication regimen closely tend to experience smoother recoveries. Avoiding strenuous activity, rubbing the eye, and exposure to dust or water also helps protect healing during this sensitive first week.

How Does Vision Improve Between One and Four Weeks Post-Surgery?
Vision improves between one and four weeks post-surgery as inflammation subsides and the eye adjusts to the new intraocular lens. Most patients experience meaningful gains in clarity and sharpness throughout this period.
Clinical data indicates that vision typically begins to improve within the first week, with many patients resuming driving within one to two weeks once vision has stabilized and been cleared by a surgeon. By the end of the first month, the majority of patients notice a significant difference in everyday tasks, such as reading signs, watching television, and recognizing faces at a distance.
During this phase, mild fluctuations in visual acuity remain normal. The brain also needs time to neuroadapt to the new lens, particularly with multifocal or extended depth of focus designs. Consistent use of prescribed drops and attendance at scheduled follow-up appointments help ensure steady progress throughout this critical recovery window.
When Does Vision Fully Stabilize After Cataract Surgery?
Vision fully stabilizes after cataract surgery for most patients between four and eight weeks, though some individuals may notice subtle refinements for up to three months. The exact timeline depends on the type of intraocular lens implanted, pre-existing eye conditions, and individual healing rates.
According to a report from the American Academy of Ophthalmology’s IRIS registry, 81.7% of 33,437 eyes achieved a corrected distance visual acuity of 20/40 or better by postoperative month one. This threshold represents functional vision sufficient for most daily activities, including driving.
Patients with extended depth of focus or trifocal IOLs may require a longer neuroadaptation period before experiencing the full range of their new lens capabilities. Those with pre-existing conditions, such as mild macular changes or dry eye, should anticipate a more gradual stabilization curve. A final refraction assessment, typically performed four to six weeks after surgery, determines whether updated glasses are needed for any residual prescription.
With a clear understanding of recovery milestones, recognizing common visual symptoms during healing becomes the next important step.
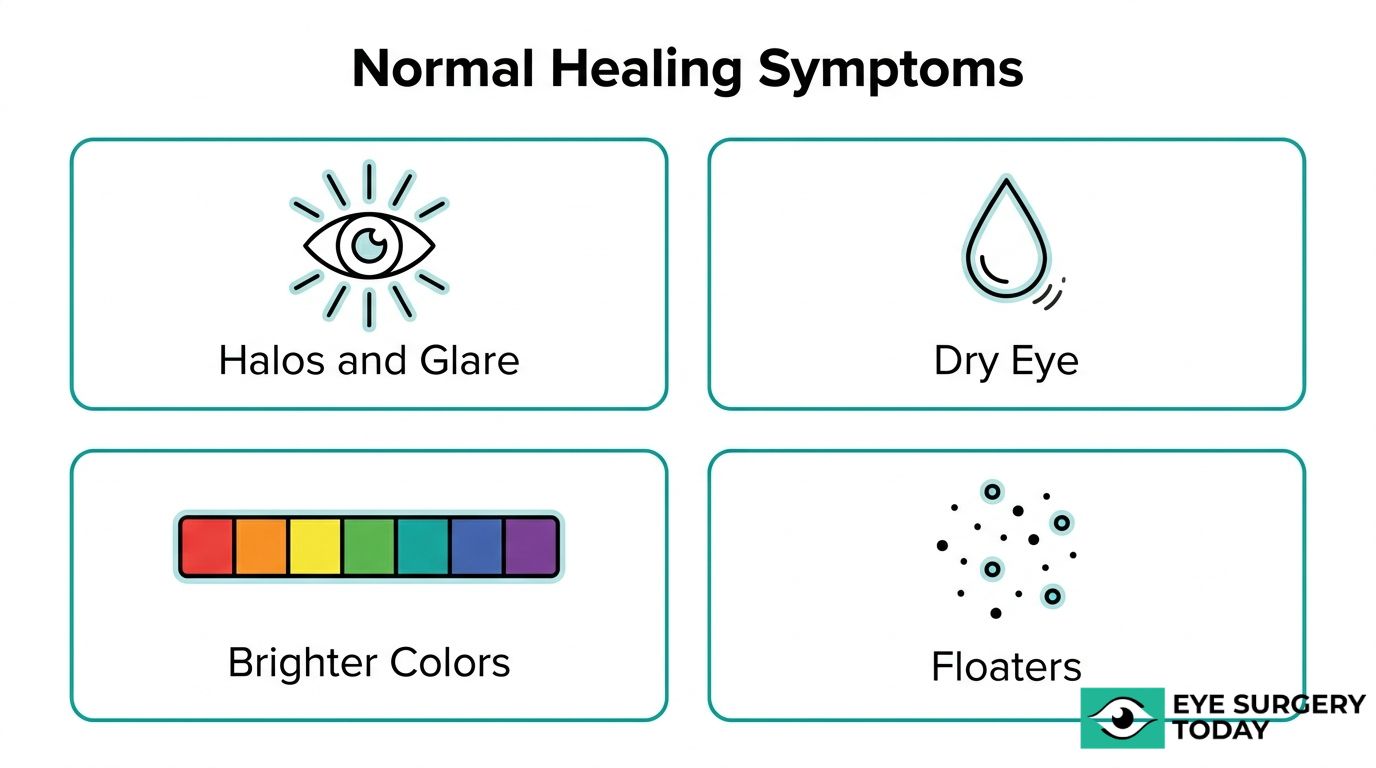
What Are Common Visual Symptoms During Cataract Surgery Recovery?
Common visual symptoms during cataract surgery recovery include halos, glare, dry eye, brighter color perception, and floaters. The sections below explain why each symptom occurs and when it typically resolves.
Why Do Halos and Glare Occur After Cataract Surgery?
Halos and glare occur after cataract surgery because the eye is adjusting to the new intraocular lens (IOL) while mild corneal swelling and residual inflammation alter how light refracts. The edge design of the IOL can scatter incoming light, producing rings around light sources at night and increased sensitivity to bright environments. These visual phenomena are especially common during the first few weeks, when the cornea and pupil are still healing. According to clinical guidelines referenced by the American Academy of Ophthalmology, the initial postoperative examination should typically occur within 24 hours to monitor for intraocular pressure spikes and early complications that could worsen such symptoms. For most patients, halos and glare diminish significantly as inflammation subsides and the brain adapts to the new lens optics over several weeks.
What Causes Dry Eye Symptoms After Cataract Surgery?
Dry eye symptoms after cataract surgery are caused by disruption of the corneal nerve plexus during the incision, reduced tear film stability, and inflammation of the ocular surface. The phacoemulsification procedure and use of a lid speculum can temporarily decrease corneal sensitivity, which slows the natural blink reflex and reduces tear production. Preservatives in postoperative eye drops may further irritate the surface. According to a study published in PLOS One, the incidence of dry eye after phacoemulsification was found to be 9.8%, with symptoms appearing as early as seven days post-surgery and typically resolving or stabilizing by three months. Patients who had pre-existing dry eye before surgery may experience more pronounced discomfort. Preservative-free artificial tears and consistent use of prescribed anti-inflammatory drops can help manage symptoms during this recovery window.
Why Do Colors Look Brighter After Cataract Surgery?
Colors look brighter after cataract surgery because the clouded natural lens, which previously filtered and yellowed incoming light, has been replaced with a clear artificial IOL. Over years, a cataract gradually shifts color perception toward warmer, muted tones. Most patients do not notice this change until the lens is removed. Once the clear IOL is in place, the full visible light spectrum reaches the retina without obstruction, making blues, greens, and whites appear noticeably more vivid. This enhanced color perception is one of the most immediate and positive changes patients report. While the brightness can feel intense at first, the visual system typically adjusts within a few days to weeks as the brain recalibrates to unfiltered light input.
What Causes Floaters After Cataract Surgery?
Floaters after cataract surgery are caused by small clumps of collagen fibers or cells within the vitreous humor that cast shadows on the retina. These pre-existing floaters often become more noticeable after surgery because the clear IOL allows more light into the eye, illuminating vitreous opacities that the cataract previously obscured. In some cases, the surgical procedure itself may cause minor vitreous disturbance, temporarily increasing floater visibility. A few small, stable floaters are generally considered a normal part of recovery. However, a sudden increase in floaters, especially when accompanied by flashing lights or a curtain-like shadow across the visual field, may indicate a posterior vitreous detachment or retinal tear, which requires immediate evaluation by an ophthalmologist.
Understanding these common visual symptoms can help set realistic recovery expectations; the next step is knowing how your specific lens choice affects long-term clarity.
How Clear Will Your Vision Be After Cataract Surgery?
Vision clarity after cataract surgery depends largely on which intraocular lens (IOL) you receive. The following subsections cover what to expect from monofocal, multifocal, toric, and extended depth of focus IOLs.

What Vision Can You Expect with a Monofocal IOL?
You can expect sharp distance vision at one fixed focal point with a monofocal IOL. This lens type is the standard choice in cataract surgery, optimized for clear vision at a single distance, typically far. Most patients who receive a monofocal IOL achieve excellent corrected distance visual acuity, though reading glasses are usually still needed for close-up tasks.
One notable advantage is contrast sensitivity. According to a comparative analysis published by the American Academy of Ophthalmology, both multifocal and EDOF IOLs lead to a reduction in contrast sensitivity compared with monofocal IOLs, although binocular contrast sensitivity may show no significant difference in some trials. This makes the monofocal lens a particularly strong option for patients who prioritize crisp, high-contrast vision for activities like night driving.
Patients with pre-existing ocular conditions may benefit most from this straightforward lens design, since visual outcomes can be more predictable when fewer optical compromises are involved.
What Vision Can You Expect with a Multifocal IOL?
You can expect vision at multiple distances with a multifocal IOL, including near, intermediate, and far. This lens uses concentric rings or zones to split light, allowing the brain to select the appropriate focal point for each task. For many recipients, this design significantly reduces dependence on reading glasses.
However, optical trade-offs exist. According to a comparative analysis published in ScienceDirect, 12% of multifocal patients reported halos and glare compared to 5% in other IOL groups. These visual phenomena tend to be most noticeable at night or around bright light sources, and they often diminish as the brain adapts over weeks to months.
Multifocal IOLs can be a practical choice for patients seeking broad spectacle independence, but candidacy screening matters. Individuals with macular disease or significant dry eye may find these side effects more pronounced, making a thorough preoperative evaluation essential.
What Vision Can You Expect with a Toric IOL?
You can expect corrected astigmatism and improved uncorrected distance vision with a toric IOL. This lens is specifically designed with built-in cylindrical correction that neutralizes corneal astigmatism, a condition where the cornea’s irregular curvature causes blurred or distorted images at all distances.
Unlike standard monofocal lenses, toric IOLs address both the cataract and the astigmatism simultaneously during a single procedure. Precise surgical alignment is critical; even slight rotation of the lens can reduce its corrective effectiveness. For this reason, advanced imaging and careful preoperative measurements guide the surgeon’s placement.
Patients with moderate to high corneal astigmatism who choose a non-toric lens often remain dependent on glasses or contact lenses for clear distance vision. The toric IOL eliminates much of that residual blur, making it one of the most efficient ways to address astigmatism at the time of cataract removal.
What Vision Can You Expect with an Extended Depth of Focus IOL?
You can expect a continuous range of clear vision from distance through intermediate with an extended depth of focus (EDOF) IOL. Rather than splitting light into distinct focal points like a multifocal lens, the EDOF design elongates the single focus, creating a smooth transition across viewing distances.
This optical approach tends to produce fewer halos and glare complaints than multifocal IOLs, though some reduction in contrast sensitivity compared to monofocal lenses may still occur. Near vision for fine print often requires supplemental reading glasses, since the EDOF’s strongest performance falls in the distance-to-intermediate range.
For patients who spend significant time on computers or dashboards and want reduced spectacle dependence without the visual phenomena associated with multifocal designs, the EDOF IOL represents a practical middle ground. Discussing lifestyle priorities with your eye surgeon can help determine whether this lens best matches your daily visual demands.
Understanding how each IOL type shapes your postoperative clarity can help guide conversations about whether glasses may still be necessary.
Will You Still Need Glasses After Cataract Surgery?
Whether you still need glasses after cataract surgery depends on the type of intraocular lens (IOL) implanted and your individual visual needs. The sections below cover when reading glasses, distance glasses, or reduced glasses dependence may apply.
When Might You Still Need Reading Glasses After Surgery?
You might still need reading glasses after surgery if you receive a standard monofocal IOL set for distance vision. Monofocal lenses focus at one fixed point, so while they can deliver sharp distance clarity, they do not adjust for close-up tasks. Activities like reading books, viewing a phone screen, or threading a needle typically require supplemental reading glasses with this lens type.
Patients who had good near vision before surgery sometimes find this adjustment surprising. The natural lens, even when clouded by a cataract, still provided some accommodative range that a fixed-focus implant does not replicate. For anyone who prioritizes near vision, discussing premium IOL alternatives with a surgeon before the procedure can help set realistic expectations.
When Might You Still Need Distance Glasses After Surgery?
You might still need distance glasses after surgery if your IOL is set for near or intermediate focus, or if residual refractive error remains after healing. Pre-existing corneal astigmatism that is not corrected during surgery can also leave distance vision slightly blurred without corrective lenses.
Even with a distance-targeted monofocal IOL, small post-surgical refractive surprises occasionally occur. Factors such as corneal healing variability and lens positioning within the eye can shift the final focus point. In most cases, a mild glasses prescription resolves this easily. Your surgeon may recommend waiting until vision fully stabilizes, often around four to six weeks, before finalizing any new prescription.
Can Lens Choice Reduce Your Dependence on Glasses?
Yes, lens choice can reduce your dependence on glasses significantly. Multifocal, extended depth of focus (EDOF), and toric IOLs each address specific vision needs that a standard monofocal lens cannot.
Key options that may reduce glasses use include:
- Multifocal IOLs split light into multiple focal points, providing near, intermediate, and distance vision in one lens.
- EDOF IOLs elongate the range of focus, offering strong intermediate and distance vision with less reliance on reading glasses.
- Toric IOLs correct pre-existing corneal astigmatism, sharpening uncorrected distance vision for patients who would otherwise need glasses for astigmatism.
As Dr. Eric D. Donnenfeld, MD, a clinical professor of ophthalmology at NYU, emphasizes, “asking questions is a great way to get the information you need” when evaluating elective lens technology. No single IOL eliminates glasses for every situation, but the right match between lens design and lifestyle priorities can meaningfully reduce daily dependence.
With glasses expectations clarified, understanding potential risks helps complete the picture of post-surgical vision.
What Are the Possible Risks That Could Affect Vision After Cataract Surgery?
The possible risks that could affect vision after cataract surgery include posterior capsule opacification, cystoid macular edema, infection, and IOL displacement. Each complication has distinct warning signs and treatment options.
What Is Posterior Capsule Opacification?
Posterior capsule opacification (PCO) is a gradual clouding of the thin membrane left behind the intraocular lens after cataract surgery. PCO develops when residual lens epithelial cells migrate and proliferate across the posterior capsule, scattering light before it reaches the retina. This condition may cause symptoms similar to the original cataract, such as blurred vision, glare sensitivity, and difficulty reading fine print.
PCO affects up to 50% of people within two to five years post-cataract surgery, making it the most common reason for blurred vision long after the procedure. Although sometimes called a “secondary cataract,” PCO is not a new cataract forming. A YAG laser capsulotomy can treat it in a painless, outpatient procedure that typically restores clarity within days. Because PCO onset is gradual, patients often mistake it for normal aging rather than a treatable complication. Recognizing these symptoms early and reporting them to a surgeon can lead to a straightforward correction.
What Are the Signs of Cystoid Macular Edema After Surgery?
The signs of cystoid macular edema (CME) after surgery include blurred or distorted central vision, difficulty reading, and a washed-out appearance to colors. CME occurs when fluid accumulates in the macula, the part of the retina responsible for sharp central vision, typically appearing within the first few weeks to months after cataract removal.
According to data cited in the American Academy of Ophthalmology’s Preferred Practice Pattern, CME incidence rates in patients without specific risk factors range from 1% to 3.5% across various large-scale clinical studies. Patients with diabetes or a history of uveitis may face higher risk. Anti-inflammatory eye drops, including NSAIDs and corticosteroids, are commonly prescribed to manage CME, and most cases resolve with treatment. Persistent or untreated CME, however, can lead to lasting central vision loss, so any new distortion or blurriness developing weeks after surgery warrants prompt evaluation.
How Could Infection or Endophthalmitis Affect Post-Surgery Vision?
Infection or endophthalmitis could affect post-surgery vision by causing severe intraocular inflammation that damages delicate retinal and other ocular structures. Endophthalmitis is a rare but serious bacterial or fungal infection inside the eye that can develop within days of cataract surgery.
Warning signs include rapidly worsening vision, increasing eye pain, significant redness, and swollen eyelids. The overall incidence rate of acute-onset endophthalmitis after cataract surgery is approximately 0.04% to 0.2%, with modern surgical protocols and prophylactic antibiotics helping keep rates low. Despite its rarity, endophthalmitis is considered an ophthalmic emergency. Treatment typically involves intravitreal antibiotic injections, and in severe cases, a vitrectomy may be necessary. Delayed treatment significantly raises the risk of permanent vision loss. Any sudden onset of pain combined with declining vision in the first week after surgery should be treated as urgent and reported to the surgical team immediately.
What Is a Dislocated or Misaligned IOL?
A dislocated or misaligned IOL is an intraocular lens that has shifted from its intended position inside the eye after cataract surgery. The lens may decenter slightly within the capsular bag or, in rarer cases, dislocate entirely into the vitreous cavity.
Symptoms can include:
- Blurred or double vision that does not improve with glasses
- Visible edge glare or crescent-shaped shadows in peripheral vision
- Fluctuating visual clarity, especially with head movement
IOL displacement may result from weakened zonular fibers, trauma to the eye, or progressive capsular bag contraction over time. Patients with pseudoexfoliation syndrome or connective tissue disorders face elevated risk. Minor misalignment sometimes requires only monitoring and updated corrective lenses, while significant dislocation typically requires surgical repositioning or lens exchange. A large multicenter study in the United Kingdom found that over 95% of eyes with no ocular comorbidity achieved corrected distance visual acuity of 20/40 or better, underscoring that complications like IOL displacement remain uncommon when the eye is otherwise healthy. Promptly reporting any visual disturbance helps preserve the best possible outcome.
Understanding these risks prepares patients to recognize warning signs that benefit from timely medical attention.
When Should You Contact Your Doctor About Vision After Cataract Surgery?
You should contact your doctor about vision after cataract surgery when you notice sudden changes suggesting complications or gradual shifts that may indicate a treatable issue. The sections below cover urgent symptoms and slower-developing changes worth reporting.
What Sudden Vision Changes Require Immediate Medical Attention?
Sudden vision changes that require immediate medical attention include a rapid loss of vision, intense eye pain, significant increase in floaters, flashes of light, or a curtain-like shadow across your visual field. These symptoms can signal serious complications such as retinal detachment, acute endophthalmitis, or a sudden rise in intraocular pressure.
According to the American Academy of Ophthalmology, clinical guidelines recommend that the initial postoperative examination after cataract surgery should typically occur within 24 hours to monitor for intraocular pressure spikes and early complications. If any of the following develop between scheduled visits, seek care immediately:
- A sudden, severe decline in vision that was previously improving
- New onset of intense redness, swelling, or discharge
- A dramatic increase in floaters accompanied by light flashes
- Persistent, worsening eye pain unresponsive to prescribed drops
Even when a symptom seems minor, erring on the side of caution with post-surgical eye health is always the safer approach. Delaying evaluation of acute symptoms can allow treatable conditions to progress.

What Gradual Vision Changes Should You Report to Your Surgeon?
Gradual vision changes you should report to your surgeon include a slow return of blurriness, increasing difficulty with reading or night driving, and a progressive haze that develops weeks to months after surgery. These patterns often point to conditions that respond well to treatment when identified early.
Posterior capsule opacification is one of the most common causes. According to Medical News Today, PCO affects up to 50% of people within two to five years post-cataract surgery, causing a gradual clouding that mimics the original cataract. A quick in-office YAG laser capsulotomy can typically restore clarity.
Other changes worth discussing at your next follow-up include:
- A slow increase in halos or glare around lights
- Persistent dryness that worsens rather than improves over weeks
- Subtle distortion or waviness in central vision
Not every gradual shift signals a problem; some fluctuation is part of the normal healing arc. However, consistently worsening symptoms beyond the expected recovery window deserve professional evaluation to rule out treatable conditions.
Knowing which symptoms to watch for helps you protect your visual results long after surgery day.
Who May Not Achieve Ideal Vision After Cataract Surgery?
Patients with pre-existing eye conditions, systemic health issues, or postoperative compliance challenges may not achieve ideal vision after cataract surgery. The following sections cover how conditions such as corneal astigmatism, macular degeneration, and glaucoma can affect outcomes.
How Do Pre-Existing Eye Conditions Affect Visual Outcomes?
Pre-existing eye conditions affect visual outcomes by limiting the eye’s ability to fully benefit from cataract removal alone. Corneal astigmatism, for example, can reduce uncorrected distance acuity if left unaddressed during surgery. Clinical assessments published in the American Academy of Ophthalmology find that toric IOLs are effective at correcting pre-existing corneal astigmatism and providing good uncorrected distance visual acuity compared to non-toric options.
Conditions such as diabetic retinopathy, corneal scarring, or optic nerve damage may place a ceiling on achievable clarity regardless of lens choice. Postoperative medication compliance also plays a significant role; patients who miss prescribed eye drops or do not follow discharge instructions tend to experience poorer results. For patients with known ocular comorbidities, a thorough preoperative evaluation helps set realistic expectations and guide IOL selection.
How Does Macular Degeneration Limit Results After Surgery?
Macular degeneration limits results after surgery by compromising the central retina’s ability to process fine detail, even when the new intraocular lens transmits light clearly. Because age-related macular degeneration (AMD) affects the macula rather than the lens, replacing a clouded lens cannot restore the retinal function that AMD has already reduced.
However, the outlook is more encouraging than many patients expect. According to the American Academy of Ophthalmology’s Preferred Practice Pattern, patients with AMD show substantial improvements in visual acuity after cataract surgery, and there is no evidence that surgery accelerates AMD progression. Peripheral vision and overall brightness perception often improve significantly. For individuals managing both cataracts and AMD, surgery can still meaningfully enhance quality of life, even if reading-level sharpness remains limited.
How Does Glaucoma Affect Vision Expectations After Surgery?
Glaucoma affects vision expectations after surgery by causing irreversible damage to the optic nerve, which limits the visual information that reaches the brain. Cataract surgery can improve clarity by removing the clouded lens, but it cannot restore nerve fibers already lost to glaucomatous damage. Patients with advanced glaucoma may notice improved brightness and contrast yet still experience peripheral vision gaps or reduced overall acuity.
In many cases, cataract surgery can actually lower intraocular pressure modestly, which may benefit glaucoma management. Still, the degree of pre-existing optic nerve damage largely determines the visual ceiling a patient can reach. Careful coordination between cataract and glaucoma treatment plans is essential. Patients managing both conditions should discuss realistic visual goals with their eye care provider before proceeding.
With an understanding of how pre-existing conditions shape outcomes, proactive steps during recovery can help protect and maximize your visual results.
What Can You Do to Support the Best Vision Outcome After Cataract Surgery?
You can support the best vision outcome after cataract surgery by following post-operative instructions carefully and attending all scheduled follow-up appointments. These two factors directly influence how well and how quickly your vision recovers.
Which Post-Operative Instructions Matter Most for Recovery?
The post-operative instructions that matter most for recovery are medication compliance, activity restrictions, and eye protection protocols. Your surgeon will typically prescribe antibiotic and anti-inflammatory eye drops on a specific schedule; using them exactly as directed helps prevent infection and control swelling during the critical early healing window.
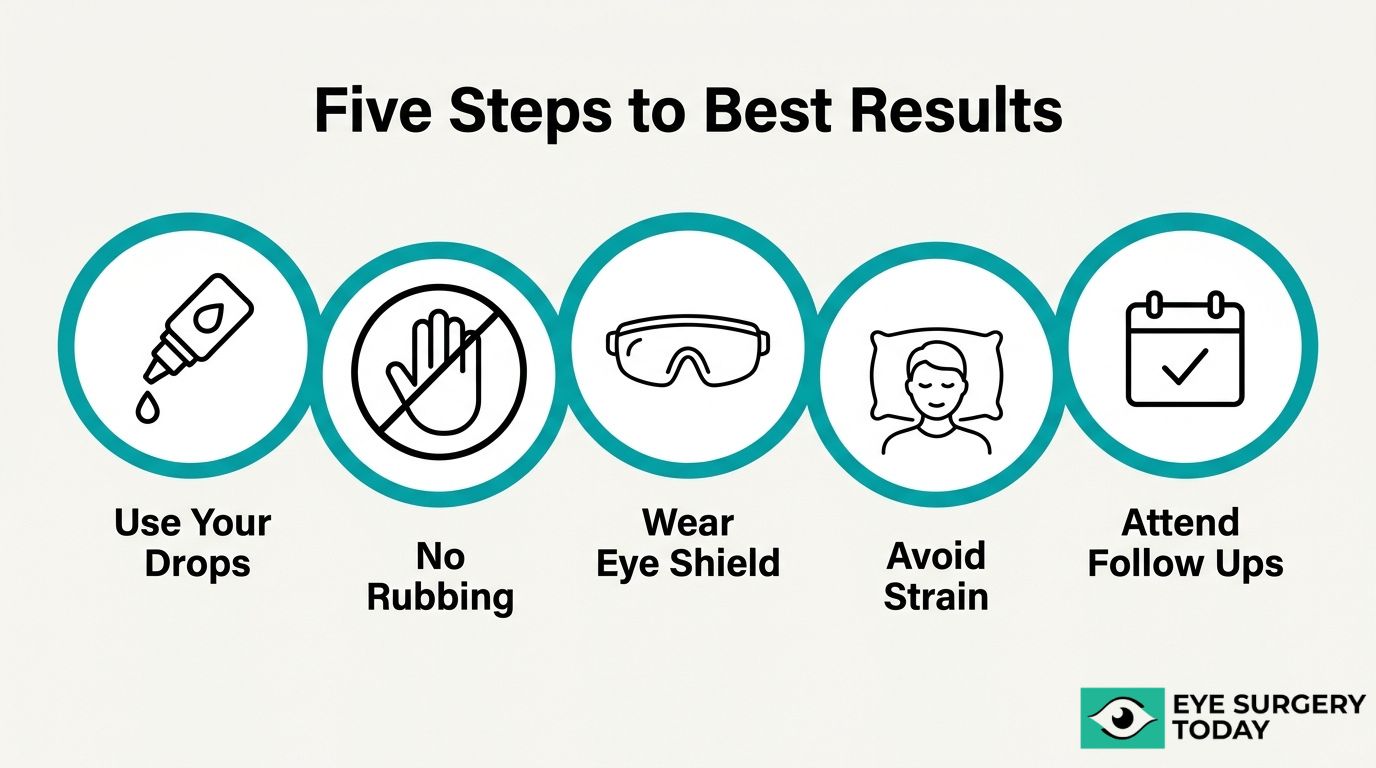
Key post-operative instructions include:
- Follow your eye drop schedule precisely. Skipping doses or stopping early can increase the risk of inflammation or infection.
- Avoid rubbing or pressing on the operated eye. Even gentle pressure can disturb the healing incision or shift the newly placed IOL.
- Wear your protective eye shield while sleeping. This prevents accidental contact with the eye during the first week.
- Avoid heavy lifting, bending, and strenuous exercise. These activities can raise intraocular pressure and compromise healing.
- Keep water, soap, and dust away from the eye. Contamination during early recovery is a preventable cause of complications.
Noncompliance with postoperative medication regimens significantly correlates with poorer visual outcomes and patient dissatisfaction, according to clinical data published on medRxiv. Patients who understand their instructions before leaving the surgical center tend to follow them more consistently, which is why asking questions before discharge can make a meaningful difference in recovery quality.
How Do Follow-Up Appointments Protect Your Visual Results?
Follow-up appointments protect your visual results by allowing your surgeon to detect and address complications before they affect long-term vision. These visits typically begin within 24 hours of surgery, when monitoring for intraocular pressure spikes and early signs of infection is most critical.
During subsequent visits, your surgeon evaluates healing progress, checks IOL positioning, and adjusts your medication regimen as needed. This ongoing monitoring is especially important because some complications, such as cystoid macular edema or posterior capsule opacification, can develop weeks or months after the procedure. Early detection through follow-up care often means simpler, more effective treatment.
For patients who received premium lenses, follow-up assessments also help confirm that the chosen IOL is delivering the expected visual performance. In a comparative study published in the Journal of Refractive Surgery, patients with EDOF and trifocal IOLs achieved similar visual results, and both groups performed better than monofocal IOL recipients in terms of spectacle independence. These outcomes depend partly on post-surgical fine-tuning that only happens when patients keep their appointments.
With proper post-operative habits in place, surgeon-reviewed resources can further prepare you for each stage of recovery.
How Can Surgeon-Reviewed Resources Help You Prepare for Vision After Cataract Surgery?
Surgeon-reviewed resources can help you prepare for vision after cataract surgery by providing clinically accurate, easy-to-understand information about lens options, recovery timelines, and realistic visual expectations.
Can Eye Surgery Today Help You Understand Your IOL Options?
Yes, Eye Surgery Today can help you understand your IOL options through surgeon-reviewed educational guides that break down the differences between monofocal, multifocal, toric, and extended depth of focus lenses. Each IOL type offers distinct visual trade-offs in areas such as distance clarity, near vision, spectacle independence, and potential side effects like halos or glare. Navigating these choices without clear, unbiased information can feel overwhelming, especially when the decision directly affects daily activities like reading and driving. Eye Surgery Today translates complex clinical details into accessible language so patients can have more productive conversations with their surgical teams. The platform also offers exclusive resources, including “The Insider’s Guide to Cataract Surgery,” designed to walk patients through the decision-making process step by step.
What Are the Key Takeaways About Vision After Cataract Surgery?
The key takeaways about vision after cataract surgery center on setting realistic expectations and staying engaged throughout recovery. Most patients experience noticeable visual improvement within the first week, though full stabilization may take several weeks. Temporary symptoms such as blurriness, halos, dry eye, and brighter color perception are common and typically resolve on their own. IOL selection directly shapes your post-surgical visual experience; monofocal lenses optimize distance vision, while multifocal and EDOF options may reduce glasses dependence at the cost of mild contrast changes. Pre-existing conditions like macular degeneration, glaucoma, or diabetes can influence outcomes, making preoperative screening essential. Following post-operative instructions and attending all follow-up appointments remain the most reliable ways to protect your results. For patients seeking surgeon-reviewed guidance on any of these topics, Eye Surgery Today provides the clarity needed to approach cataract surgery with confidence.