Life After Cataract Surgery: Recovery, Expectations & What to Look Out For
Cataract surgery is a procedure that removes the clouded natural lens and replaces it with an artificial intraocular lens (IOL) to restore light transmission to the retina. Recovery follows a predictable pattern for most patients, though individual healing timelines vary.
This guide covers the recovery timeline and healing phases, normal postoperative side effects, care instructions and activity restrictions, potential complications and warning signs, expected vision results, and how follow-up appointments support long-term outcomes.
Most patients return to daily activities within about one week, with refraction often stabilizing by the end of that first week. Functional vision typically improves within a month, though full recovery in some cases may take up to 12 weeks as the IOL settles and the eye completes its internal healing.
Temporary side effects such as blurry vision, halos, grittiness, eye redness, and light sensitivity are common in the early weeks. These symptoms generally reflect normal postoperative swelling and incision healing rather than complications, and most resolve gradually without additional treatment.
Postoperative care involves prescribed eye drops for approximately four weeks, wearing a protective eye shield during sleep, and avoiding activities that may raise eye pressure or introduce bacteria to the healing incision. Driving, exercise, swimming, and makeup each carry specific resumption timelines based on infection risk and healing progress.
While serious complications such as endophthalmitis, posterior capsule opacification, retinal detachment, and cystoid macular edema are uncommon, recognizing their warning signs early can be critical. Sudden vision loss, worsening pain, or new flashes of light warrant immediate contact with your surgeon.
Final visual outcomes depend on the IOL type selected and individual eye health, with a follow-up visit around four to six weeks after surgery used to assess acuity and determine whether corrective lenses may still be needed.
What Does the Cataract Surgery Recovery Timeline Look Like?
The cataract surgery recovery timeline spans from the first postoperative day through several weeks, with most healing milestones occurring in defined phases. Below, each stage covers what to expect from day one through full recovery.
What Happens in the First 24 Hours After Cataract Surgery?
The first 24 hours after cataract surgery involve an initial adjustment period during which vision is typically blurry, the eye may feel slightly sore, and a protective shield is placed over the operated eye. Phacoemulsification, the modern standard for cataract surgery, uses ultrasound to break up the clouded lens before removing it through a small incision. Because this incision is minimal, early discomfort tends to be mild.
During this phase, the implanted intraocular lens (IOL) begins settling into position. According to a study published on PubMed, capsular contact with the IOL optic is completed within approximately 8 days with silicone IOLs and 11 days with acrylic IOLs. While visual improvement can be noticeable within hours, the eye remains in its most vulnerable state during this window. Patients should rest, avoid touching the eye, and attend their day-one follow-up appointment.
What Should You Expect During the First Week of Recovery?
During the first week of recovery, you should expect gradual visual improvement alongside temporary side effects, such as mild grittiness, light sensitivity, and fluctuating clarity. According to the American Academy of Ophthalmology, feeling like there is sand in the eye is a normal sensation caused by the small surgical incision, and it should heal within a week or so.
Prescribed eye drops, typically antibiotics and anti-inflammatories, are essential during this period to prevent infection and manage swelling. Most patients find that refraction begins stabilizing by the end of this first week. Avoiding heavy lifting, dusty environments, and rubbing the eye helps protect the healing incision.
How Does Your Vision Change in Weeks Two Through Four?
Your vision changes in weeks two through four as residual swelling subsides, the IOL fully stabilizes, and the brain adjusts to the new artificial lens. Colors often appear brighter and more vivid compared to the muted tones caused by the cataract. Mild fluctuations in sharpness can still occur, particularly in the morning or after extended screen use, but these episodes typically become less frequent with each passing day.
This is also the period when your ophthalmologist may evaluate whether a new glasses prescription is appropriate. For many patients, the most dramatic improvement in visual clarity becomes apparent during these weeks as the eye reaches a more settled state.
When Is Cataract Surgery Recovery Fully Complete?
Cataract surgery recovery is fully complete for most patients between 4 and 12 weeks after the procedure, depending on individual healing factors and the type of IOL implanted. According to the American Academy of Ophthalmology, improvement in visual function is typically achieved within 90 days following cataract surgery in a high percentage of patients aged 18 and older.
A follow-up visit around the 4 to 6 week mark allows your eye care provider to assess final visual acuity and determine if corrective lenses are needed. Although the eye may feel normal well before this point, the internal healing process, including complete capsular adaptation, continues quietly beneath the surface. Patience during this final phase helps ensure the best long-term outcome.
Understanding the full recovery timeline sets the stage for recognizing which postoperative symptoms are normal and which deserve closer attention.
What Are the Normal Side Effects After Cataract Surgery?
The normal side effects after cataract surgery include blurry vision, halos, glare, eye redness, grittiness, and light sensitivity. The sections below explain each one and when it typically resolves.
Is Blurry Vision Normal After Cataract Surgery?
Blurry vision is normal after cataract surgery. According to the American Academy of Ophthalmology, it is very common to have blurry or unclear vision in the days and sometimes even weeks after cataract removal, most often caused by normal swelling in the eye as part of the healing process.
This postoperative blur can feel alarming, but it reflects the eye adjusting to the new intraocular lens (IOL) while residual corneal edema subsides. Most patients regain functional vision within a month, though full recovery may take 4 to 12 weeks depending on individual healing. For patients who notice fluctuating clarity during this window, the pattern is almost always progressive improvement rather than decline. Persistent blurriness beyond several weeks, however, warrants a follow-up with your eye care provider.
Why Do You See Halos or Glare After Cataract Surgery?
You see halos or glare after cataract surgery because of a phenomenon called dysphotopsia. According to the American Academy of Ophthalmology, many cataract patients experience “unwanted visual images” after surgery, with glare, halos, and streaks of light being examples of positive dysphotopsia that occur more frequently at night or with multifocal lenses.
The edge design of the IOL can refract light in ways the natural lens did not, producing these visual artifacts. In most cases, the brain adapts over weeks to months through a process called neuroadaptation, and the symptoms become far less noticeable. Patients with multifocal IOLs may take longer to adjust than those with monofocal lenses, which is worth discussing with your surgeon before selecting a lens type.
Is Eye Redness Common After Cataract Surgery?
Eye redness is common after cataract surgery. According to the American Academy of Ophthalmology, a red or bloodshot eye after surgery, often a subconjunctival hemorrhage, is very common and harmless, typically healing on its own within two to three weeks.
This redness results from small blood vessels breaking on the surface of the eye during the procedure. While it can look dramatic, a subconjunctival hemorrhage does not affect vision or indicate a deeper problem. The body reabsorbs the blood gradually, and no treatment is usually required. If redness is accompanied by increasing pain or vision changes, your ophthalmologist may want to evaluate for other causes.
Why Does Your Eye Feel Gritty or Dry After Surgery?
Your eye feels gritty or dry after surgery because the small incision made during cataract removal temporarily disrupts the corneal surface and nerve feedback that regulate tear production. This sandy, foreign-body sensation is a normal part of early recovery and typically resolves within a week or so as the incision heals.
Preservative-free artificial tears can help manage dryness during this period. Patients who had pre-existing dry eye disease before surgery may notice these symptoms lasting longer, making it especially important to discuss dry eye management with your doctor during postoperative visits.
Is Light Sensitivity Expected After Cataract Surgery?
Light sensitivity is expected after cataract surgery. Mild photophobia commonly occurs because the new IOL allows more light into the eye than the clouded natural lens did, and postoperative dryness can intensify the sensation.
Wearing sunglasses outdoors during the first few weeks helps reduce discomfort while the eye adjusts. However, the American Academy of Ophthalmology notes that extreme light sensitivity can be a sign of inflammation, known as iritis, or infection. If photophobia worsens rather than gradually improves, or is accompanied by deep eye pain, contacting your eye care provider promptly is important to rule out complications.
Understanding which side effects are routine helps you focus on recovery with confidence rather than unnecessary worry.
What Post-Operative Care Instructions Should You Follow?
The post-operative care instructions you should follow include using prescribed eye drops on schedule, wearing a protective eye shield while sleeping, and keeping the area around your eye clean without letting water or pressure touch it directly.

Which Eye Drops Are Prescribed After Cataract Surgery?
The eye drops prescribed after cataract surgery typically include three categories: antibiotic drops to prevent infection, anti-inflammatory drops to control swelling, and steroid drops to support healing. According to the NHS, patients are usually given eye drops for about 4 weeks after cataract surgery to help the eye heal and prevent infection.
Your ophthalmologist may provide a specific dosing schedule that tapers over those four weeks. Following the prescribed timing matters, since skipping doses or stopping early can increase the risk of inflammation or bacterial complications. If you use multiple drop types, waiting at least five minutes between each one allows proper absorption. Consistent use of post-operative eye drops is one of the simplest yet most impactful steps patients can take during the recovery period.
How Should You Protect Your Eye While Sleeping?
You should protect your eye while sleeping by wearing the plastic eye shield your surgeon provides, typically for at least the first week after surgery. The shield prevents accidental rubbing, pressure from pillows, or contact with bedding that could disturb the healing incision.
Most surgeons recommend taping the shield securely over the operated eye each night before bed. Sleeping on your back or on the side opposite the treated eye can further reduce the chance of inadvertent contact. Even if the eye feels comfortable after a few days, continuing to wear the shield for the full recommended period helps safeguard against bumps or unconscious touching during sleep.
How Should You Clean Around Your Eye After Surgery?
You should clean around your eye after surgery using a damp, clean cloth or sterile gauze, gently wiping the surrounding skin without touching the eye itself. Key precautions include:
- Avoid letting tap water, soap, or shampoo contact the operated eye directly.
- Do not rub or apply pressure to the eye or eyelid.
- Use a fresh cloth each time to minimize infection risk.
- Clean from the inner corner outward with light, single-stroke motions.
If discharge or crustiness accumulates along the lash line, your surgeon may recommend using cooled boiled water on a cotton pad. Keeping the area clean without introducing contaminants supports smooth healing during those critical first weeks.
Understanding how to care for your eye at home sets a strong foundation before reviewing which activities to avoid during recovery.
What Activities Should You Avoid During Recovery?
You should avoid activities that increase infection risk, raise eye pressure, or irritate the healing incision during cataract surgery recovery. The subsections below cover driving, exercise, showering, work, swimming, and makeup timelines.

When Can You Drive After Cataract Surgery?
You can drive after cataract surgery once your surgeon confirms adequate visual acuity, which typically takes a few days to one week. According to the Vision Institute, most surgeons advise patients to avoid driving for at least a few days after surgery, and sometimes for a week or two, depending on individual recovery. Depth perception and light sensitivity may still be adjusting during this window, making it unsafe to operate a vehicle. Your ophthalmologist will assess your vision at the first follow-up visit before clearing you to drive.
When Can You Exercise After Cataract Surgery?
You can exercise after cataract surgery once enough time has passed for the incision to stabilize, though the timeline depends on exercise intensity. Light activities, such as gentle walking, can typically resume within a few days. Strenuous activities and heavy lifting should be avoided for at least two weeks following surgery to ensure safe recovery, as recommended by the Pacific Eye Institute. Bending at the waist, straining, or lifting heavy objects may increase intraocular pressure, which can compromise the healing incision. Your surgeon will provide specific clearance based on your individual progress.
When Can You Shower or Wash Your Hair After Surgery?
You can shower after cataract surgery within the first day or two, but you should take precautions to keep water, soap, and shampoo out of the operated eye. Tilting your head back while washing your hair helps prevent water from running directly into the eye. For the first one to two weeks, avoiding direct water pressure on the face reduces the risk of introducing bacteria to the healing incision. A clean washcloth can be used to gently clean around the eye without touching it directly.
When Can You Return to Work After Cataract Surgery?
You can return to work after cataract surgery within approximately one week for most desk-based or low-physical-demand jobs. According to Moorfields Eye Hospital NHS Foundation Trust, it usually takes around one week to get back to day-to-day activities, although recovery time varies from person to person. Jobs requiring heavy lifting, exposure to dust, or strenuous physical labor may require a longer absence of two weeks or more. Discussing your specific work environment with your surgeon helps determine the safest timeline.
When Is It Safe to Swim After Cataract Surgery?
It is safe to swim after cataract surgery once at least two weeks have passed, provided there are no complications. According to the American Academy of Ophthalmology, doctors advise swimmers to wait at least two weeks before going in the water to minimize the risk of infection and irritation. Pools, hot tubs, lakes, and oceans all carry bacteria that can enter the eye through the healing incision. This two-week minimum aligns with the broader recovery milestone; spectacle prescriptions can also safely be provided around this timeframe following uncomplicated surgery. Wearing goggles when resuming swimming offers an additional layer of protection.
When Can You Wear Makeup After Cataract Surgery?
You can wear makeup after cataract surgery once your surgeon confirms sufficient healing, which is typically two weeks after the procedure. Eye makeup, such as mascara, eyeliner, and eyeshadow, poses a particular risk because particles can migrate into the eye and introduce bacteria. Face makeup applied away from the eye area may be safe sooner, but caution is still warranted. Replacing old eye cosmetics with new products before resuming use reduces contamination risk. For most patients, this two-week restriction aligns with the general activity resumption timeline.
With activity restrictions clear, knowing which warning signs require medical attention keeps recovery on track.
What Are the Possible Risks and Complications to Watch For?
The possible risks and complications to watch for after cataract surgery include infection, posterior capsule opacification, retinal detachment, sudden vision loss, increased eye pressure, and cystoid macular edema.
What Are the Signs of Infection After Cataract Surgery?
The signs of infection after cataract surgery include increasing pain, worsening redness, swelling of the eyelid, discharge, and a noticeable decline in vision. Endophthalmitis, the most serious form of post-surgical eye infection, can develop within the first few days. Symptoms may escalate rapidly, making early detection critical.
If you notice any combination of these warning signs, especially pain that intensifies rather than improves, contact your eye surgeon immediately. Prompt treatment with antibiotics can help preserve vision when infection is caught early. Most ophthalmologists consider any new or worsening symptom in the first week a reason for urgent evaluation.
What Is Posterior Capsule Opacification?
Posterior capsule opacification (PCO) is a condition where the thin membrane behind the intraocular lens becomes cloudy after cataract surgery, causing vision to gradually blur again. According to a study published in Clinical Ophthalmology, PCO incidence ranged from 10.5% to 42.9% in studies of high myopic patients following cataract surgery.
PCO can be treated with a YAG laser capsulotomy, a quick and safe laser procedure that restores clear vision. The treatment takes only a few minutes and is performed in an office setting. Because PCO develops gradually over months or years, many patients initially mistake the symptoms for their cataract returning. Recognizing that this is a treatable and common occurrence can save unnecessary worry.
What Does Retinal Detachment Feel Like After Surgery?
Retinal detachment after cataract surgery may feel like a sudden increase in floaters, flashes of light, or a shadow or curtain moving across your field of vision. According to a study published in PubMed, the risk for rhegmatogenous retinal detachment after phacoemulsification is small, but younger patients face a higher risk for pseudophakic detachment.
These symptoms can appear suddenly and without pain, which makes them easy to dismiss. Any new onset of flashes, a shower of floaters, or peripheral vision loss warrants immediate medical attention. Early surgical intervention can help reattach the retina and preserve sight.
What Should You Do if You Experience Sudden Vision Loss?
If you experience sudden vision loss after cataract surgery, you should contact your eye surgeon or go to an emergency room immediately. Sudden loss of vision can indicate serious complications, such as endophthalmitis, retinal detachment, or a significant rise in intraocular pressure.
Do not wait to see if symptoms improve on their own. Time-sensitive intervention may be necessary to prevent permanent damage. While rare, these emergencies require professional evaluation within hours rather than days. Keeping your surgeon’s emergency contact information readily accessible during recovery is one of the most practical steps you can take.
Can Increased Eye Pressure Occur After Cataract Surgery?
Yes, increased eye pressure can occur after cataract surgery. A temporary spike in intraocular pressure (IOP) may develop within the first 24 hours or during the early recovery period. Causes include residual viscoelastic material from surgery, inflammation, or steroid eye drops used during recovery.
According to a report published by the National Institutes of Health, routine postoperative follow-up in the United States typically occurs on day 1, one week, and one month after cataract surgery to monitor healing and visual outcomes. These scheduled visits allow your surgeon to detect elevated eye pressure before it causes harm. Patients with a history of glaucoma may face a higher risk and should discuss monitoring plans with their surgical team beforehand.
What Is Cystoid Macular Edema After Cataract Surgery?
Cystoid macular edema (CME) is a common complication following cataract surgery that causes transient blurred vision due to fluid accumulation in the macula, the central part of the retina responsible for sharp vision. According to a report published in JAMA, CME is recognized as one of the most frequent causes of reduced vision after otherwise successful cataract procedures.
Symptoms typically appear weeks after surgery and include blurry or distorted central vision. Anti-inflammatory eye drops, including nonsteroidal anti-inflammatory drugs (NSAIDs), can help manage and resolve the condition. In most cases, CME responds well to treatment, though persistent cases may require additional intervention. For patients noticing a gradual decline in clarity after an initially successful recovery, CME is one of the first conditions an ophthalmologist will evaluate.
Understanding these potential complications prepares you to recognize warning signs and seek timely care.
When Should You Call Your Doctor After Cataract Surgery?
You should call your doctor after cataract surgery if you experience sudden vision loss, severe eye pain, increasing redness, flashes of light, a curtain-like shadow in your vision, or signs of infection such as thick discharge or swelling that worsens rather than improves.
While mild discomfort, light sensitivity, and blurry vision are expected during the first few days of recovery, certain symptoms can signal complications that require prompt medical attention. Knowing the difference between normal healing and a potential problem helps you act quickly when it matters.
Contact your ophthalmologist right away if you notice any of the following:
- Sudden, significant vision loss in the operated eye, which may indicate retinal detachment, endophthalmitis, or a spike in intraocular pressure.
- Intense or worsening eye pain that does not respond to prescribed drops or over-the-counter pain relief, as this can suggest inflammation or infection.
- Increasing redness that spreads or deepens after the first few days, rather than gradually fading as expected with a normal subconjunctival hemorrhage.
- Flashes of light or new floaters, especially a sudden shower of floaters, which may be associated with retinal detachment.
- A shadow or curtain moving across any part of your visual field, another possible sign of retinal detachment requiring urgent evaluation.
- Thick or colored discharge from the eye, particularly if accompanied by swelling of the eyelid, as these symptoms may point to endophthalmitis or another infection.
- Extreme light sensitivity that worsens instead of improving. According to the American Academy of Ophthalmology, while some light sensitivity after cataract removal is expected due to dryness, extreme sensitivity can be a sign of inflammation (iritis) or infection.
- Persistent nausea or vomiting following surgery, which may be related to elevated eye pressure.
Most of these complications are rare; however, early detection significantly improves outcomes. Routine postoperative follow-up in the United States typically occurs on day one, one week, and one month after surgery to monitor healing. Between those visits, do not wait for your next scheduled appointment if any of these warning signs appear. A brief phone call to your surgeon’s office can determine whether you need to be seen sooner.
In clinical practice, patients who report symptoms early tend to have better outcomes than those who assume discomfort will resolve on its own. When in doubt, contacting your eye care provider is always the safer choice.
Understanding which symptoms warrant a call prepares you to recognize what your post-surgical vision results may look like as healing progresses.
What Vision Results Can Cataract Surgery Potentially Provide?
Cataract surgery can potentially provide significantly improved visual clarity, though final results depend on the intraocular lens (IOL) selected and individual eye health. The subsections below cover achievable clarity and whether glasses may still be needed.
How Clear Can Your Vision Become After Cataract Surgery?
Your vision can become substantially clearer after cataract surgery, with most patients noticing a meaningful improvement once the eye fully heals. The clouded natural lens is replaced with an artificial IOL, which restores light transmission to the retina. According to Moorfields Eye Hospital, it usually takes around one week to get back to day-to-day activities after cataract surgery, though visual sharpness continues to refine over the following weeks.
The degree of clarity depends on several factors:
- The type of IOL implanted (monofocal, multifocal, or extended depth of focus).
- Pre-existing conditions such as macular degeneration or glaucoma.
- The accuracy of preoperative biometry measurements.
A follow-up appointment at around four weeks is necessary to assess the final visual outcome. For patients without other eye conditions, modern IOL technology can deliver crisp, high-contrast vision that many describe as better than what they experienced for years before surgery.
Will You Still Need Glasses After Cataract Surgery?
Whether you will still need glasses after cataract surgery depends primarily on the IOL type implanted. Monofocal IOLs, the most commonly used lens, excel at providing sharp distance vision but typically require reading glasses for close-up tasks. Multifocal and extended depth of focus IOLs can achieve a higher degree of spectacle independence by addressing multiple focal distances, though they may introduce subtle visual trade-offs such as mild halos.
According to World Health Organization practice guidelines, a follow-up visit four to six weeks after surgery is recommended to evaluate visual acuity and address the need for refractive correction. This appointment determines the final spectacle prescription, if one is needed.
In clinical practice, most patients find their dependence on glasses is significantly reduced regardless of IOL choice. Discussing lifestyle priorities with your eye surgeon before surgery remains the most reliable way to match lens selection with your daily visual needs.
How Do Follow-Up Appointments Support Your Recovery?
Follow-up appointments support your recovery by allowing your ophthalmologist to monitor healing, detect complications early, and determine when your vision has stabilized enough for a final prescription. These visits follow a structured schedule designed to track each phase of the healing process.
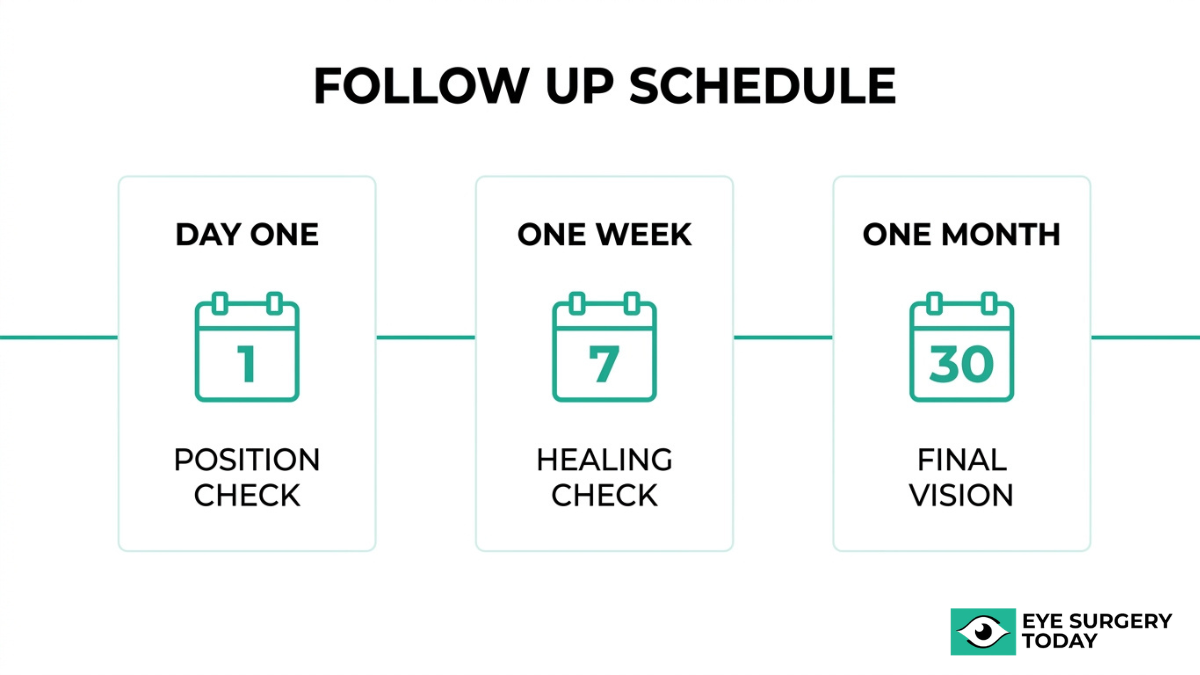
Routine postoperative follow-up in the United States typically occurs on day 1, one week, and one month after cataract surgery, according to a study published in the National Institutes of Health (PMC). Each visit serves a distinct clinical purpose:
- Day-one visit confirms the intraocular lens is properly positioned and checks for early signs of infection or elevated eye pressure.
- One-week visit evaluates initial healing, assesses whether inflammation is resolving, and adjusts eye drop regimens if needed.
- One-month visit measures visual acuity, evaluates the final refractive outcome, and determines whether a spectacle prescription is appropriate.
A follow-up appointment at around four weeks is particularly important because it allows your surgeon to assess the final visual outcome and provide a definitive spectacle prescription. Skipping this visit can delay the detection of conditions like posterior capsule opacification or cystoid macular edema, both of which respond well to treatment when caught early. For patients who experience no complications, these three visits are often sufficient to confirm a successful recovery. Understanding what each appointment evaluates can help you prepare questions and recognize whether your healing is progressing as expected, which is where surgeon-reviewed resources become especially valuable.
How Can Surgeon-Reviewed Resources Help You Navigate Recovery?
Surgeon-reviewed resources can help you navigate recovery by providing clinically accurate, easy-to-understand guidance at every stage of healing. The sections below cover how Eye Surgery Today supports your understanding and the key takeaways from this article.
Can Eye Surgery Today Help You Understand Your Recovery?
Yes, Eye Surgery Today can help you understand your recovery by offering surgeon-reviewed educational content that translates complex post-operative information into clear, actionable guidance. The platform was built by nationally recognized ophthalmology key opinion leaders specifically to bridge the knowledge gap many cataract patients face.
Every article, guide, and resource on Eye Surgery Today goes through a surgeon review process to ensure clinical accuracy. Rather than relying on generic health content, patients gain access to the same quality of insight that informed surgical professionals use, presented in language anyone can follow. Eye Surgery Today also provides resources covering IOL options, recovery timelines, and post-operative care instructions, so patients can revisit reliable information between follow-up appointments. For those preparing for surgery or currently recovering, this kind of trustworthy, unbiased education can reduce uncertainty and support more confident decision-making.
What Are the Key Takeaways About Life After Cataract Surgery?
The key takeaways about life after cataract surgery center on realistic expectations, consistent post-operative care, and knowing when to seek help. Recovery follows a predictable pattern for most patients, though individual timelines vary:
- Most patients return to daily activities within about one week, with functional vision typically restored within a month.
- Normal side effects, such as blurry vision, mild grittiness, light sensitivity, and eye redness, usually resolve within the first few weeks.
- Prescribed eye drops, activity restrictions, and proper eye protection are essential during the initial healing window.
- Serious complications like endophthalmitis, retinal detachment, and cystoid macular edema are uncommon but require immediate attention if warning signs appear.
- Follow-up appointments at key intervals allow your surgeon to monitor healing, check visual acuity, and determine when a final spectacle prescription is appropriate.
Understanding what is normal and what warrants a call to your doctor is one of the most valuable things a patient can take away from their pre-surgical research. With the right preparation and access to surgeon-reviewed resources like those on Eye Surgery Today, patients can approach recovery with greater confidence and fewer surprises.
