Cataracts: Early Symptoms, Diagnosis, and How They Affect Your Vision
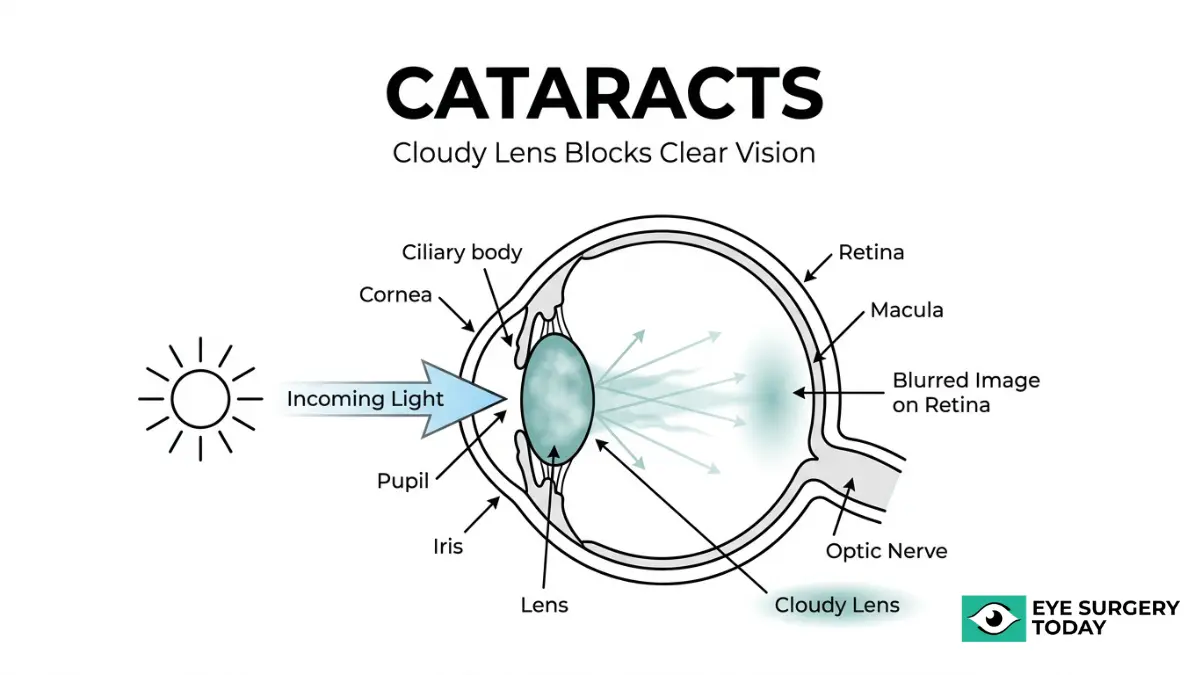
A cataract is a cloudy area in the eye’s lens that forms when proteins break down and clump together, scattering incoming light instead of focusing it clearly on the retina. This protein aggregation typically begins around age 40, though noticeable vision changes may not appear for years or even decades.
This guide covers early symptom recognition, cataract types and their causes, clinical diagnosis methods, vision progression over time, and strategies for prevention and informed decision-making.
Early cataracts can produce blurry vision, increased glare sensitivity, halos around lights, fading colors, frequent prescription changes, and monocular double vision. Because these changes develop gradually, many people compensate without realizing their lens is clouding.
Cataracts are classified into several types, including nuclear sclerotic, cortical, posterior subcapsular, congenital, and traumatic, each forming in a distinct part of the lens and producing different symptom patterns. Aging, oxidative stress, UV exposure, diabetes, smoking, and prolonged corticosteroid use are all associated with accelerated lens clouding.
The gold standard for diagnosis is a comprehensive dilated eye exam using slit-lamp biomicroscopy, supplemented by visual acuity testing and retinal imaging. These evaluations assess not only lens clarity but also functional impact on daily activities like driving and reading.
As cataracts progress from early to advanced stages, they may impair independence; however, unlike glaucoma or macular degeneration, cataracts can be surgically treated by replacing the clouded lens with a clear intraocular lens. Understanding symptoms, risk factors, and diagnostic options early can support timely evaluation and more confident conversations with your eye care provider.
What Is a Cataract and What Happens Inside the Eye?
A cataract is a cloudy area in the lens of the eye that forms when proteins in the lens break down and clump together. The lens, normally clear, sits behind the iris and focuses light onto the retina to produce sharp images. When these structural proteins aggregate, they scatter incoming light instead of transmitting it cleanly, which progressively reduces visual clarity.
This process typically begins around age 40, though noticeable vision changes may not appear for years. According to the National Eye Institute, the protein breakdown that initiates lens clouding is a normal part of aging, with clumping gradually increasing over time. Oxidative stress plays a central role in this process; when the lens’s natural antioxidant defenses weaken, reactive oxygen species damage both proteins and lipid structures within the lens microenvironment.
As clouding spreads, the lens loses its ability to refract light accurately. Colors may appear faded, bright lights can produce glare or halos, and fine detail becomes harder to distinguish. The degree of visual disruption depends on the cataract’s size, density, and location within the lens. A small opacity near the periphery may go unnoticed for years, while clouding in the central visual axis can impair sight much earlier.
What makes cataracts particularly deceptive is their gradual onset. Many people unknowingly compensate by increasing lighting or holding reading material closer, delaying recognition of the underlying cause. Understanding this internal process is the first step toward recognizing early symptoms and seeking timely evaluation.
What Are the Early Symptoms of Cataracts?
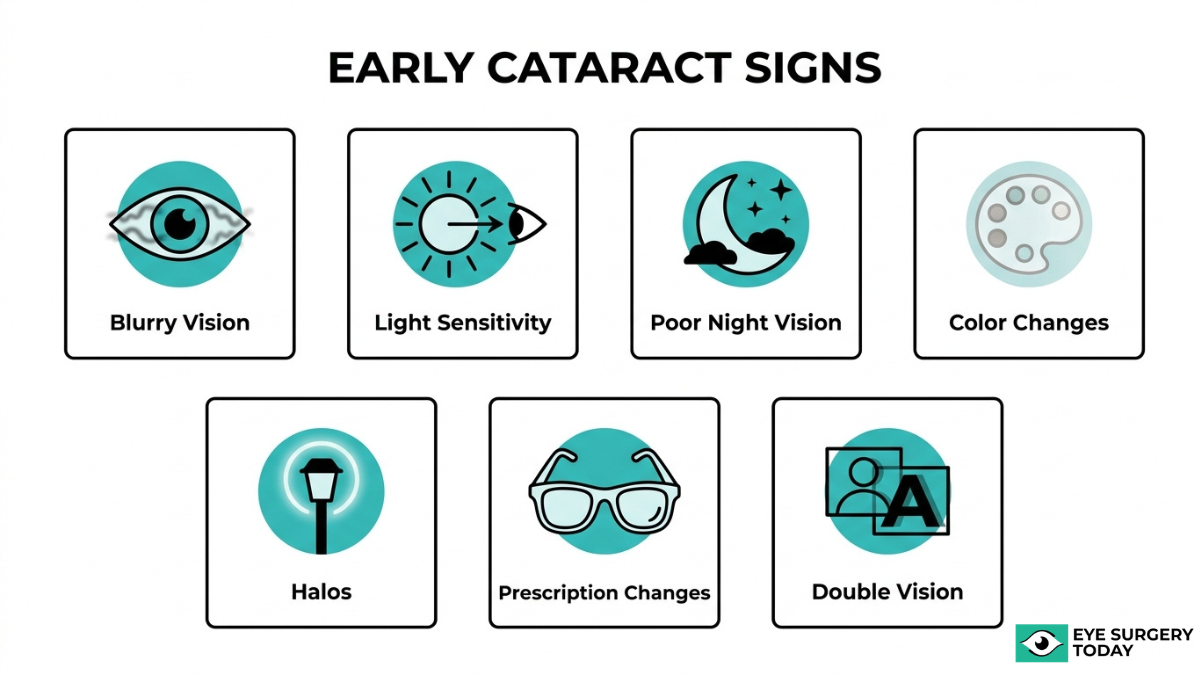
The early symptoms of cataracts include blurry vision, light sensitivity, poor night vision, color changes, halos, shifting prescriptions, and monocular double vision.
How Does Blurry or Cloudy Vision Present in Early Cataracts?
Blurry or cloudy vision presents in early cataracts as a gradual haziness that affects part or all of the visual field. As lens proteins begin to clump together, small areas of opacity form that scatter incoming light before it reaches the retina. Initially, the cloudiness may be so subtle that it resembles looking through a slightly fogged window. Many people compensate without realizing it by using brighter lights or holding reading material closer. Because the progression is slow, this symptom often goes unnoticed until a routine eye exam reveals measurable changes in visual clarity. Blurry vision from early cataracts tends to worsen in low-contrast settings, making it harder to distinguish edges and fine details.
How Do Cataracts Cause Increased Sensitivity to Light and Glare?
Cataracts cause increased sensitivity to light and glare because the clouded lens scatters light rather than focusing it clearly on the retina. This scattering sends unfocused rays across the visual field, producing a washed-out or dazzling effect.
The type of cataract determines how glare manifests:
- Cortical cataracts appear as wedge-shaped opacities that begin at the outer edge of the lens and progress toward the center, frequently causing significant glare.
- Posterior subcapsular cataracts form at the back of the lens directly in the path of light, often progressing more rapidly than other types and causing severe glare along with reading difficulties.
According to the Mayo Clinic, these structural differences explain why some patients experience debilitating glare while others notice only mild discomfort. For many individuals, oncoming headlights at night become one of the first triggers that prompt an eye exam. In clinical practice, glare severity is one of the most reliable early indicators that a cataract is beginning to interfere with daily function.
How Do Cataracts Affect Your Night Vision?
Cataracts affect night vision by reducing the amount of light that passes clearly through the lens, making dim environments especially difficult to navigate. When light is already limited, even a mild opacity can significantly degrade contrast and clarity.
Halos around streetlights and oncoming headlights become more pronounced in darkness, and depth perception may diminish. According to the World Health Organization, cataracts are the leading cause of distance vision impairment globally, affecting approximately 94 million people as of 2026. Difficulty driving at dusk or nighttime is often the first functional limitation patients report. This symptom deserves particular attention because it carries real safety consequences that extend beyond simple visual discomfort.
How Do Cataracts Cause Fading or Yellowing of Colors?
Cataracts cause fading or yellowing of colors as the lens progressively absorbs short-wavelength light, making blues and purples appear dull while whites take on a yellowish tint. This shift happens so gradually that many people do not recognize the change until after cataract surgery restores normal color perception.
Nuclear sclerotic cataracts are the primary type responsible for this effect. They involve a gradual yellowing and hardening of the central lens nucleus, which acts like a tinted filter over the visual field. The color distortion can affect everyday tasks, from matching clothing to interpreting traffic signals. This is one of the more underestimated early symptoms because the brain adapts to the gradual color shift, masking the extent of the change.
How Do Cataracts Create Halos Around Lights?
Cataracts create halos around lights when the clouded lens diffracts incoming light rays, spreading them into concentric rings rather than allowing a sharp focal point. This optical effect is most noticeable around bright point-light sources, such as streetlamps, headlights, and overhead fixtures.
Halos may appear as bright circles with soft, glowing edges. Although halos can occur with other conditions, their presence alongside other symptoms on this list strongly suggests cataract involvement. Night driving tends to make this symptom most apparent, as multiple bright light sources create overlapping halos that reduce overall visual clarity.
How Do Cataracts Lead to Frequent Changes in Eyeglass Prescriptions?
Cataracts lead to frequent changes in eyeglass prescriptions because the lens opacity alters the eye’s refractive properties as it progresses. The shifting density and shape of the clouded lens changes how light bends before reaching the retina, causing measurable shifts in nearsightedness or farsightedness.
A pattern of prescription updates every few months, rather than the typical one to two years, can be an early clinical signal. Each new prescription may provide temporary improvement, but the underlying cataract continues to evolve. When an optometrist notices rapid, unexplained refractive changes in a patient over 50, cataract evaluation is typically the next step.
How Does Double Vision in One Eye Indicate a Cataract?
Double vision in one eye, known as monocular diplopia, indicates a cataract when the clouded lens splits incoming light rays into separate paths. Unlike binocular double vision caused by eye alignment issues, monocular diplopia persists even when the unaffected eye is closed.
This symptom occurs because irregular areas of opacity within the lens create multiple focal points. The result is a ghost image or shadow overlapping the primary image. Monocular diplopia from cataracts is distinct and diagnostically useful because most other causes of double vision involve both eyes working together.
What Is Second Sight and Why Does It Occur with Cataracts?
Second sight is a temporary improvement in near vision that occurs with cataracts, specifically nuclear sclerotic cataracts. As the central lens nucleus hardens and becomes denser, it increases the eye’s refractive power, effectively creating a stronger natural magnifying effect.
Patients who previously relied on reading glasses may find they can suddenly read without them. While this can feel like a welcome change, it signals advancing cataract development rather than genuine visual improvement. The effect is short-lived; as the cataract progresses further, both near and distance vision deteriorate. Recognizing second sight for what it is helps prevent delays in seeking a comprehensive eye evaluation.
With these early symptoms identified, understanding the different types of cataracts clarifies why each symptom pattern varies.
What Are the Different Types of Cataracts?
The different types of cataracts are nuclear sclerotic, cortical, posterior subcapsular, congenital, traumatic, and secondary cataracts. Each type forms in a distinct part of the lens and produces different visual symptoms.
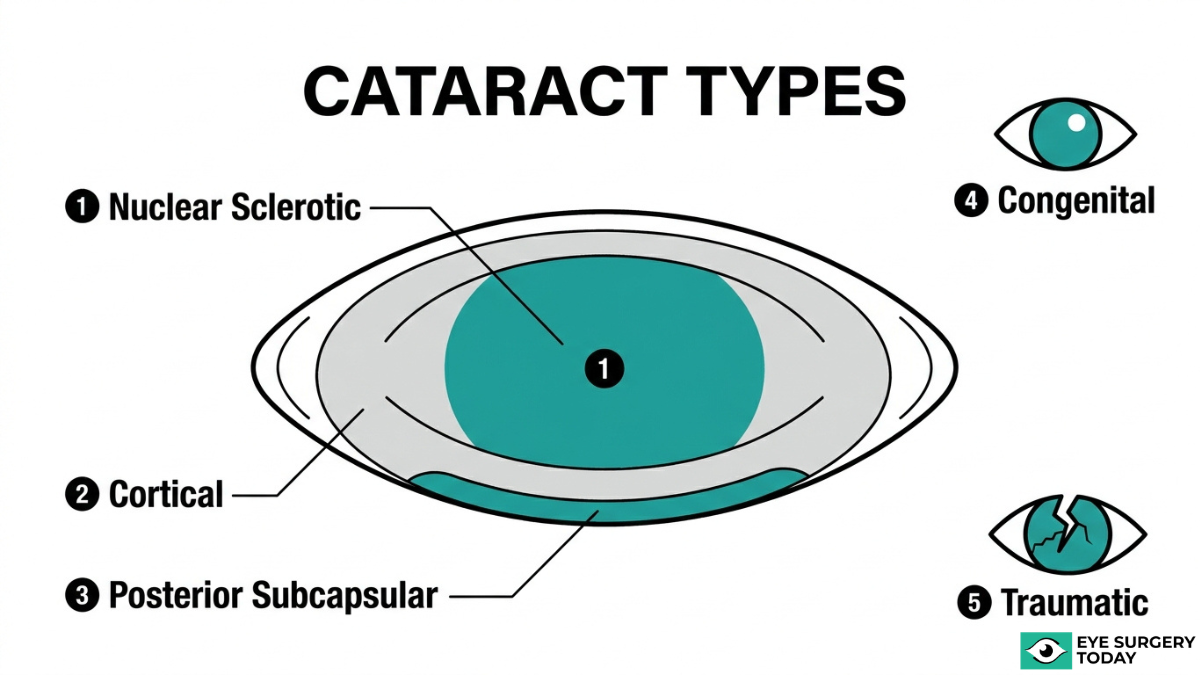
Nuclear Sclerotic Cataract
A nuclear sclerotic cataract is a gradual yellowing and hardening of the central lens nucleus. This is the most common age-related cataract type, developing slowly over years. According to the American Academy of Ophthalmology, nuclear sclerotic cataracts can cause a temporary improvement in near vision known as “second sight,” which occurs as the hardening lens briefly enhances its focusing power. Despite this short-lived benefit, the nucleus continues to darken over time. Colors may appear increasingly washed out or tinted yellow-brown, and distance vision progressively worsens. Because changes happen so gradually, many people do not notice significant vision loss until the cataract reaches a moderate or advanced stage.
Cortical Cataract
A cortical cataract forms in the outer edge, or cortex, of the lens. Wedge-shaped opacities, often described as white “spokes,” begin at the lens periphery and extend inward toward the center. This spoke-like pattern scatters incoming light before it reaches the retina, which is why cortical cataracts frequently cause significant glare. Bright sunlight and oncoming headlights at night can become particularly bothersome. As the spokes grow and converge, they increasingly interfere with both distance and near vision. Cortical cataracts are commonly associated with diabetes and prolonged ultraviolet light exposure, making UV-protective eyewear one of the simplest preventive measures available.
Posterior Subcapsular Cataract
A posterior subcapsular cataract forms at the back surface of the lens, directly in the path of light entering the eye. This positioning causes severe glare and reading difficulties, and these cataracts often progress more rapidly than nuclear or cortical types. According to a study published in Clinical & Experimental Ophthalmology, prolonged use of corticosteroids, whether topical, systemic, or inhaled, specifically promotes posterior subcapsular cataract formation. UV radiation also contributes by generating free radicals that damage lens proteins. Because of the fast progression and significant impact on close-up tasks, posterior subcapsular cataracts tend to be diagnosed in younger, more symptomatic patients compared to other types.
Congenital Cataract
A congenital cataract is a lens opacity present at birth or developing during early childhood. These cataracts may be unilateral or bilateral and vary widely in size and visual impact. Maternal infections during pregnancy, such as rubella and rubeola, are closely associated with congenital cataract formation, as are metabolic disorders affecting fetal development. Early detection is critical because an untreated congenital cataract can lead to amblyopia, or “lazy eye,” by depriving the developing visual system of clear input. Pediatric ophthalmologists typically assess the need for IOL implants and surgical intervention based on the cataract’s density, location, and effect on the child’s visual development.
Traumatic Cataract
A traumatic cataract results from physical injury to the eye. Blunt force trauma, penetrating injuries, and even electric shock can all damage the lens structure, leading to opacity. Blunt trauma characteristically produces a rosette-shaped cataract pattern, while penetrating injuries may cause more irregular opacification. These cataracts can develop immediately after the injury or appear months to years later. Traumatic cataracts are the most common cause of unilateral lens opacification in young individuals, making them particularly important to monitor after any significant eye injury.
Secondary Cataract
A secondary cataract, also called posterior capsule opacification, develops after cataract surgery when residual lens epithelial cells proliferate across the posterior capsule. Although not technically a new cataract, it produces similar symptoms: blurry vision, glare, and difficulty reading. Secondary cataracts can also refer to lens opacities caused by other medical conditions or treatments, such as diabetes or radiation therapy. Treatment is straightforward; a YAG laser capsulotomy creates an opening in the clouded capsule, restoring clear vision in a brief outpatient procedure. Knowing how cataracts are classified helps clarify the underlying causes that drive their development.
What Causes Cataracts to Develop?
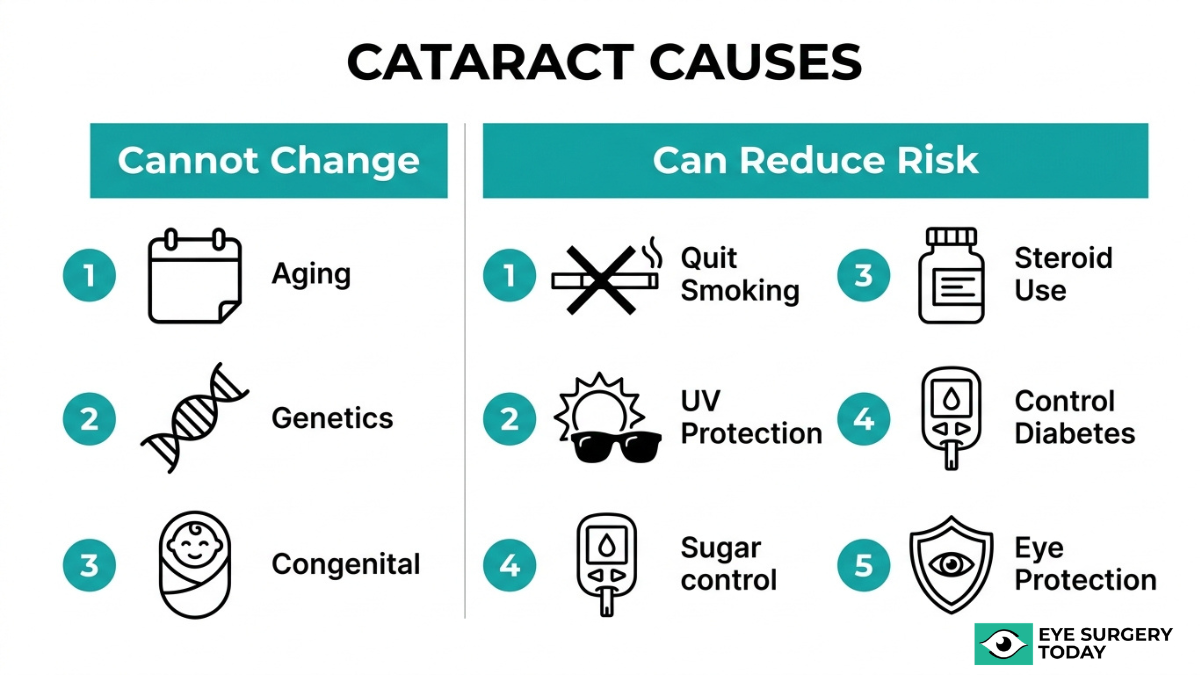
Cataracts develop when proteins inside the eye’s natural lens break down and clump together, creating cloudy areas that block light. The causes range from aging and oxidative damage to systemic diseases and environmental exposure.
Aging is the most common cause. According to the National Eye Institute, proteins in the lens begin to break down and clump together around age 40, though visible symptoms may not appear for years. These early molecular changes, known as post-translational modifications of crystallin proteins, occur long before any opacity becomes noticeable.
Oxidative stress plays a central role in this process. Defects in the lens’s antioxidative defense systems allow reactive oxygen species to accumulate, triggering protein aggregation and lipid deterioration within the lens. Several factors accelerate this damage:
- Ultraviolet radiation generates free radicals that cause oxidative damage to lens epithelial cells and structural proteins, particularly promoting cortical and posterior subcapsular opacities.
- Diabetes mellitus may increase cataract risk approximately twofold due to sorbitol accumulation in the lens, which causes osmotic overhydration.
- Prolonged corticosteroid use, whether topical, systemic, or inhaled, specifically promotes posterior subcapsular cataract formation.
- Smoking increases oxidative stress while reducing protective antioxidant levels in the lens.
- Eye trauma from blunt force, penetrating injury, or electric shock can cause traumatic cataracts, often appearing as rosette-shaped opacities.
- Congenital factors, including maternal infections such as Rubella or metabolic disorders during fetal development, may lead to cataracts present at birth.
What makes cataract development particularly challenging to detect early is that the biochemical changes precede any visual symptoms by years, sometimes decades. This is why routine eye exams remain essential even when vision feels normal. Understanding your individual risk factors can help guide how frequently you and your eye care provider should monitor for lens changes.
Who Is Most at Risk for Developing Cataracts?
The people most at risk for developing cataracts include older adults, smokers, individuals with diabetes, those with prolonged corticosteroid use, and people with significant UV exposure. While aging remains the primary driver, several modifiable and non-modifiable factors can accelerate lens clouding.
Key risk factors include:
- Advanced age. Lens proteins begin to break down and clump together around age 40, with risk increasing significantly each decade after.
- Smoking. Tobacco use increases oxidative stress and depletes protective antioxidants in the lens. According to a study published in the British Journal of Ophthalmology, smoking is a significant modifiable risk factor for cataract development.
- Diabetes. Elevated blood sugar may promote sorbitol accumulation in the lens, leading to osmotic changes that accelerate clouding.
- Prolonged corticosteroid use. Long-term use of topical, systemic, or inhaled corticosteroids can promote posterior subcapsular cataract formation.
- UV radiation exposure. Cumulative ultraviolet light exposure generates free radicals that damage lens proteins over time.
- Eye trauma. Previous injury to the eye can cause localized lens opacification, sometimes years after the initial event.
Among these, smoking and UV exposure stand out as the most actionable targets for risk reduction, since both can be addressed through lifestyle changes and consistent eye protection. Understanding personal risk factors is the first step toward timely diagnosis, which is covered next.
How Are Cataracts Diagnosed?
Cataracts are diagnosed through a series of specialized eye tests that evaluate lens clarity, visual function, and retinal health. The key diagnostic methods include a comprehensive dilated eye exam, slit-lamp examination, visual acuity testing, and retinal imaging.
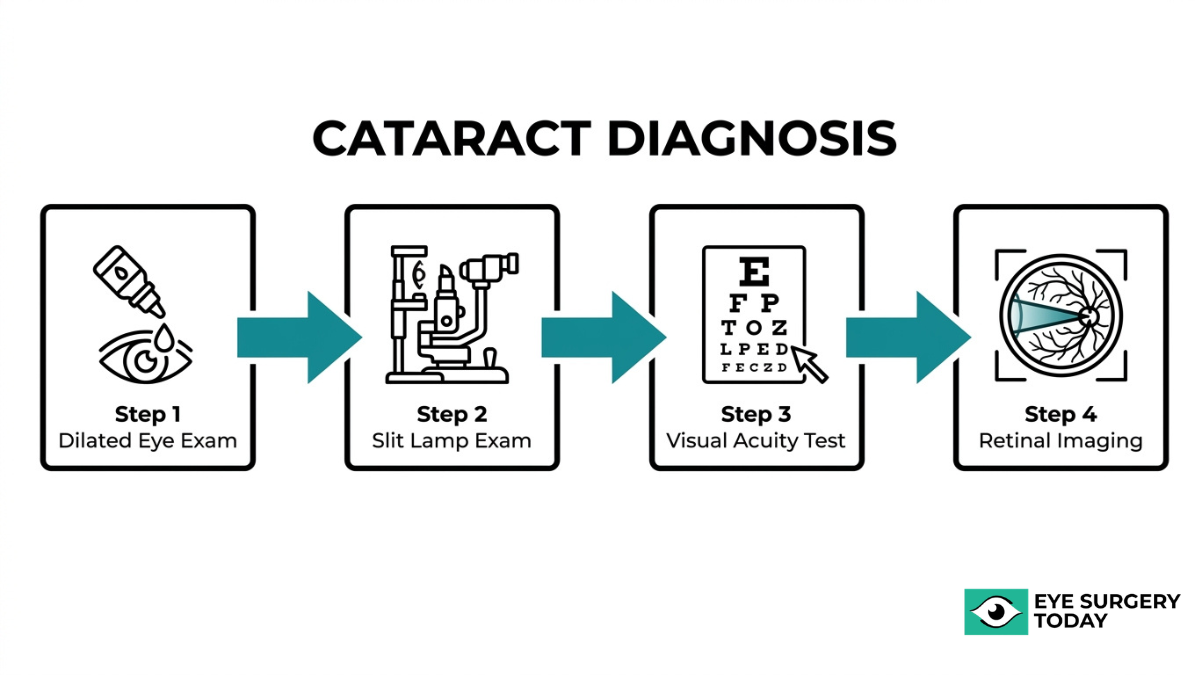
What Happens During a Comprehensive Dilated Eye Exam?
A comprehensive dilated eye exam involves your eye doctor placing special drops in your eyes to widen the pupils, allowing a detailed view of the lens and internal eye structures. Once the pupils are dilated, the doctor can examine the lens for clouding, assess the optic nerve, and check the retina for any related conditions.
According to the American Optometric Association, the gold standard for cataract diagnosis is a comprehensive dilated eye exam using slit-lamp biomicroscopy to visualize lens structures under high magnification. This exam does more than detect cataracts; it also helps rule out other conditions that may be contributing to vision changes. For most adults over 40, scheduling a dilated eye exam every one to two years can help catch lens changes before they significantly affect daily life.
What Is a Slit-Lamp Examination and How Does It Detect Cataracts?
A slit-lamp examination detects cataracts by projecting a thin, focused beam of light into the eye while the doctor views the structures through a high-powered microscope. This combination of intense light and magnification reveals the precise location, size, and density of any lens opacities.
The slit-lamp can distinguish between different cataract types, such as nuclear, cortical, or posterior subcapsular, based on where the clouding appears within the lens. Because each type affects vision differently, identifying the specific pattern of opacification helps guide treatment decisions. The narrow beam also allows the doctor to examine the lens in cross-section, making even early or subtle changes visible that a standard examination might miss.
How Does a Visual Acuity Test Help Identify Cataracts?
A visual acuity test helps identify cataracts by measuring how clearly each eye can see letters or symbols at a standardized distance. Declining acuity, particularly when corrective lenses no longer restore sharp vision, often signals lens clouding rather than a simple refractive error.
However, visual acuity alone does not capture the full impact of cataracts on everyday function. As noted in the journal Ophthalmology, functional impairment from cataracts is clinically assessed not just by visual acuity but by the patient’s ability to perform activities of daily living and their performance in glare testing. This broader evaluation matters because two patients with identical acuity scores may experience very different levels of difficulty with tasks like driving at night or reading in dim light, depending on the type and location of their cataract.
How Does Retinal Imaging Confirm Cataract Severity?
Retinal imaging confirms cataract severity by capturing detailed photographs or scans of the structures behind the lens, revealing how much the cataract obstructs the view of the retina. Technologies such as optical coherence tomography (OCT) and fundus photography allow the doctor to assess whether the retina and macula are healthy before recommending surgery.
When a cataract is dense enough to block clear retinal imaging, that obstruction itself serves as an indicator of advanced severity. Confirming retinal health before cataract surgery is essential; if an underlying retinal condition exists, it may limit the visual improvement surgery can provide. This step ensures that both the doctor and the patient have realistic expectations about outcomes.
Understanding how cataracts are diagnosed prepares you for the next important question: how they progress and affect vision over time.
How Do Cataracts Progress and Affect Vision Over Time?
Cataracts progress through distinct stages, gradually affecting daily activities, driving ability, detail work, and eventually independence. The following subsections cover each stage of functional impact.
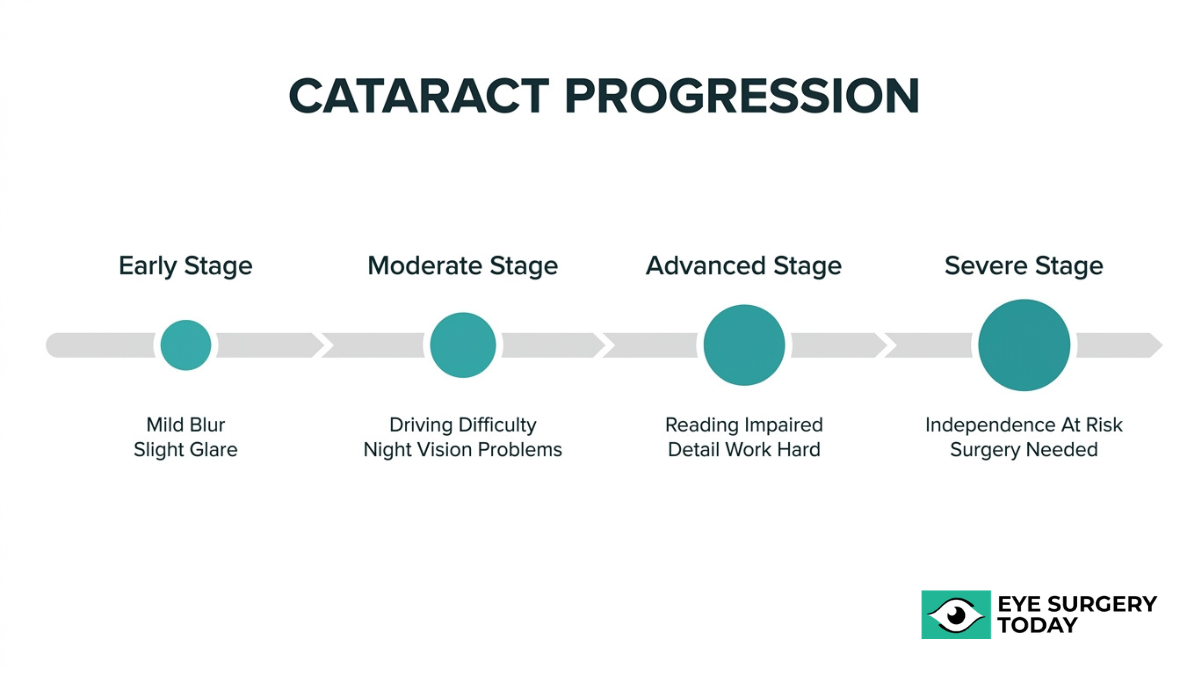
How Do Early-Stage Cataracts Affect Daily Activities?
Early-stage cataracts affect daily activities in subtle ways that are easy to dismiss. Mild lens clouding may cause slightly blurred vision, increased glare sensitivity when stepping into bright sunlight, and a faint haze over fine print. Most people at this stage can still perform routine tasks, though they may notice they need more light for reading or that colors appear slightly muted.
These early changes often go unnoticed for months or even years. Compensating with brighter lamps, adjusting screen contrast, or holding reading material at different angles can mask the gradual decline. However, these small workarounds signal that the lens is already beginning to scatter light rather than focusing it cleanly onto the retina. An updated eyeglass prescription may temporarily restore clarity at this stage, but the underlying clouding continues to progress.
How Do Moderate Cataracts Change Your Ability to Drive?
Moderate cataracts change your ability to drive by significantly increasing glare sensitivity and reducing contrast perception, particularly under low-light conditions. Oncoming headlights may scatter across the visual field, creating halos that obscure lane markings and road signs. Judging distances becomes harder as contrast between objects and their backgrounds diminishes.
According to research from the University of California, Irvine, post-translational modifications of crystallin proteins, including chemical changes that occur long before visible opacities appear, are the early molecular drivers of age-related cataract formation. By the moderate stage, these accumulated protein changes produce enough lens opacity to compromise the visual demands of safe driving. Nighttime and twilight driving typically deteriorate first, and many individuals begin avoiding highways or unfamiliar routes. For anyone noticing these changes, a comprehensive dilated eye exam can determine whether the cataract has reached a level that warrants closer monitoring or intervention.
How Do Advanced Cataracts Impact Reading and Detail Work?
Advanced cataracts impact reading and detail work by creating dense clouding that standard corrective lenses can no longer compensate for. Fine print becomes illegible, threading a needle or reading medication labels may feel impossible, and digital screens appear washed out regardless of brightness settings.
At this stage, the lens opacity blocks or distorts enough light that even well-lit environments fail to produce sharp images on the retina. Posterior subcapsular cataracts, which form directly in the light path, tend to cause especially severe reading difficulties and progress more rapidly than other types. Colors lose further distinction, with whites taking on a yellowish tint that makes it difficult to differentiate similar shades. Relying on magnification tools offers diminishing returns because the problem lies within the lens itself, not in the eye’s focusing power.
When Do Cataracts Become Severe Enough to Impair Independence?
Cataracts become severe enough to impair independence when the lens reaches a mature or near-mature stage, rendering daily self-care tasks unsafe or impractical. Navigating stairs, recognizing faces, preparing meals, and managing medications all become compromised when visual acuity drops below functional thresholds.
Clinical assessment at this stage evaluates more than a letter chart. Functional impairment from cataracts is clinically assessed not just by visual acuity but by the patient’s ability to perform activities of daily living and their performance in glare testing, according to research published in the journal Ophthalmology. When these measures confirm that vision loss meaningfully limits independence, cataract surgery typically becomes the recommended course of action. Delaying intervention at this point carries real risks, including falls, social isolation, and medication errors. Recognizing when cataracts cross this threshold is one of the most important conversations to have with an eye care provider.
Understanding how cataracts progress at each stage can help guide timely decisions about prevention strategies and treatment options.
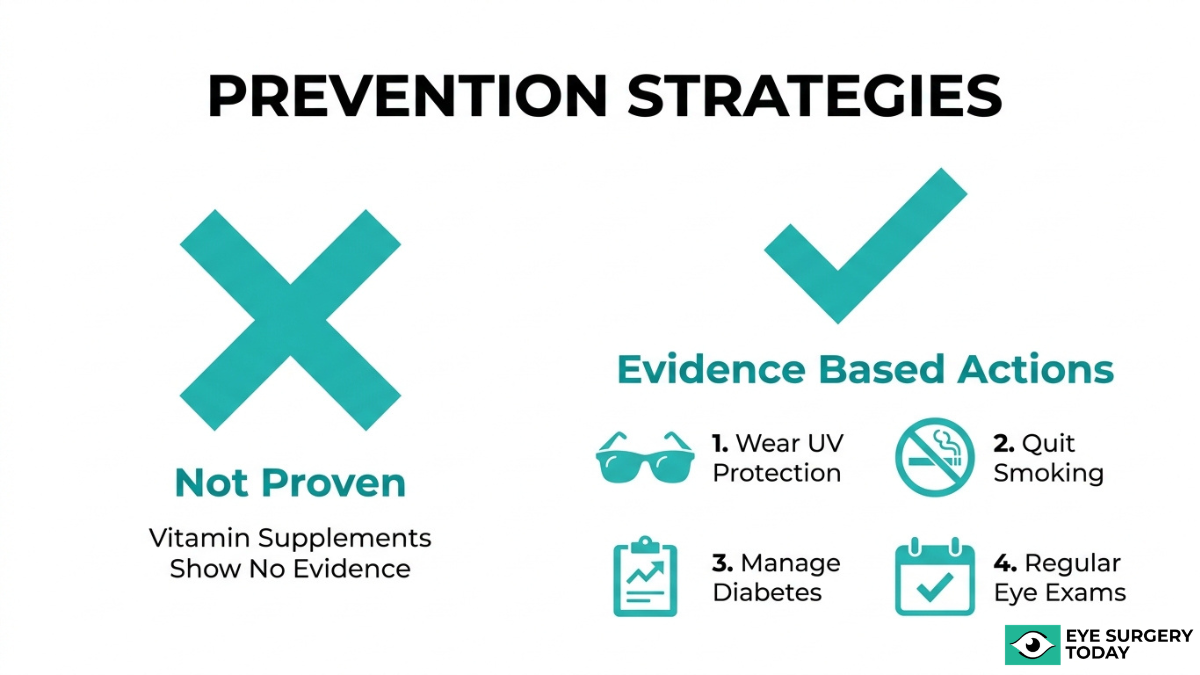
Can You Prevent Cataracts or Slow Their Progression?
You cannot fully prevent cataracts, but certain lifestyle habits may help slow their progression. No supplement has been proven to stop age-related cataracts from forming.
While the idea of a simple pill or vitamin regimen to ward off cataracts is appealing, the current body of evidence does not support that approach. According to a Cochrane Library systematic review of nine randomized controlled trials involving 117,272 participants, antioxidant vitamin supplements, including beta-carotene, vitamin C, and vitamin E, showed no evidence of preventing or slowing the progression of age-related cataracts.
That said, modifiable risk factors still matter. Steps that may help reduce cataract risk or slow progression include:
- Wearing UV-protective sunglasses to limit ultraviolet radiation exposure to the lens.
- Quitting smoking, which increases oxidative stress and depletes protective antioxidants in the lens.
- Managing underlying conditions like diabetes, which can accelerate lens changes.
- Scheduling regular comprehensive dilated eye exams to catch early lens clouding before it significantly affects vision.
Because age-related protein changes in the lens begin around age 40 and progress gradually, early detection remains the most practical strategy. No current intervention can reverse a cataract once it forms; surgery is the only definitive treatment when vision impairment affects daily life. While surgery offers significant benefits, it’s also important for patients to understand the possible complications of cataract surgery to make fully informed decisions. For most people, focusing on controllable risk factors offers more benefit than relying on supplements alone. Understanding how cataracts compare to other vision conditions can help clarify when professional evaluation is needed.
How Do Cataracts Differ from Other Common Vision Problems?
Cataracts differ from other common vision problems by affecting the lens itself, whereas conditions like glaucoma, macular degeneration, and diabetic retinopathy damage other structures of the eye. Each condition produces distinct symptoms and requires different clinical approaches.
Cataracts cause a gradual clouding of the eye’s natural lens, which scatters incoming light and reduces clarity across the entire visual field. According to the American Academy of Family Physicians, differential diagnosis of cataracts must rule out other major causes of vision loss, including glaucoma (characterized by optic nerve damage), age-related macular degeneration (central vision loss), and diabetic retinopathy (retinal vascular damage).
Key distinctions between these conditions include:
- Cataracts produce blurry or hazy vision, glare sensitivity, and color fading because the lens becomes progressively opaque.
- Glaucoma damages the optic nerve, often causing peripheral vision loss that may go unnoticed until advanced stages.
- Age-related macular degeneration targets the macula at the center of the retina, distorting or eliminating central vision while leaving peripheral sight intact.
- Diabetic retinopathy results from damage to retinal blood vessels, leading to dark spots, floaters, or sudden vision changes.
Unlike glaucoma and macular degeneration, which can cause irreversible damage, cataracts can be surgically treated by replacing the clouded lens with a clear intraocular lens. This distinction is clinically significant: while all four conditions may coexist, particularly in older adults, cataracts remain the only one where full visual restoration is routinely achievable through surgery. Recognizing which condition is responsible for vision changes is essential, since the treatment path for each differs considerably. When symptoms overlap or appear together, a comprehensive eye exam helps pinpoint the correct diagnosis and guide the right next steps.
When Should You See an Eye Doctor About Possible Cataracts?
You should see an eye doctor about possible cataracts when vision changes begin interfering with daily tasks or when you notice persistent symptoms that do not improve with updated eyeglasses.
Scheduling an eye exam is important if you experience any of the following:
- Blurry or cloudy vision that worsens gradually over weeks or months
- Increasing difficulty with nighttime driving due to glare or halos around headlights
- Colors appearing faded, washed out, or yellowish compared to how they looked before
- Frequent eyeglass or contact lens prescription changes within a short period
- Double vision in one eye that persists even when the other eye is closed
- Difficulty reading or performing detail work under normal lighting conditions
Even without noticeable symptoms, adults aged 40 and older may benefit from a baseline comprehensive dilated eye exam. According to the American Optometric Association, the gold standard for cataract diagnosis is a comprehensive dilated eye exam using slit-lamp biomicroscopy to visualize lens structures under high magnification. Because cataracts often develop slowly, early protein changes in the lens can begin long before vision feels affected.
Certain individuals should be especially proactive about scheduling an evaluation. Those with diabetes, a history of prolonged corticosteroid use, significant UV exposure, or prior eye trauma face elevated risk and may develop cataracts earlier than average. A sudden or rapid change in vision at any age warrants prompt evaluation to rule out cataracts alongside other conditions.
Waiting until cataracts severely impair independence is unnecessary. Early detection gives you and your eye care provider more time to monitor progression, adjust corrective lenses as needed, and plan for surgery when it offers the greatest benefit. Understanding your options early leads to more confident decisions about your vision care.
How Can Surgeon-Reviewed Cataract Guides Help You Understand Your Options?
Surgeon-reviewed cataract guides can help you understand your options by translating complex clinical information into clear, actionable knowledge. The sections below cover how Eye Surgery Today supports informed decision-making and the key takeaways from this article. Preparing with key questions for your cataract consultation can empower you to make the best choices for your vision.
Can Eye Surgery Today Help You Learn About Cataract Surgery?
Yes, Eye Surgery Today provides surgeon-reviewed educational guides designed to make complex eye care topics accessible. The platform provides clear, unbiased resources covering cataract symptoms, diagnosis, surgical procedures, and intraocular lens selection.
Understanding these topics matters because the decisions involved are significant. Modern cataract surgery involves the selection of an intraocular lens, with options ranging from standard monofocal lenses to advanced premium IOLs that correct for presbyopia or astigmatism. Choosing between these technologies increasingly incorporates patient lifestyle factors and healthcare cost considerations, making reliable educational resources essential. For those exploring alternatives to glasses or contacts, our resources also cover other refractive solutions like LASIK surgery and its potential benefits.
According to the National Eye Institute, more than half of all Americans age 80 or older either have cataracts or have already undergone cataract surgery. With prevalence this high, having access to trustworthy, surgeon-reviewed information empowers patients to ask better questions and participate more confidently in shared decision-making with their eye care providers.
Eye Surgery Today bridges the knowledge gap by offering guides that prioritize clarity over medical jargon, helping readers move from uncertainty to informed confidence.
What Are the Key Takeaways About Cataract Symptoms, Diagnosis, and Vision Impact?
The key takeaways about cataract symptoms, diagnosis, and vision impact are:
- Cataracts develop when proteins in the lens break down and clump together, typically beginning around age 40, and may progress gradually over years.
- Early symptoms include blurry vision, increased glare sensitivity, halos around lights, fading colors, and frequent changes in eyeglass prescriptions.
- A comprehensive dilated eye exam using slit-lamp biomicroscopy is the gold standard for cataract diagnosis.
- Cataracts progress through stages, from mild clouding with minimal impact to mature opacities that can impair driving, reading, and independence.
- Risk factors such as diabetes, prolonged corticosteroid use, smoking, and UV exposure may accelerate cataract formation.
- No current evidence supports antioxidant supplements for preventing or slowing age-related cataracts.
- Differential diagnosis should rule out glaucoma, age-related macular degeneration, and diabetic retinopathy.
Early detection remains one of the most practical steps any patient can take. Recognizing subtle changes in vision and scheduling routine eye exams allows for timely intervention before cataracts significantly affect quality of life.